VA Health Care: Opportunities Exist for VA to Better Identify and Address Racial and Ethnic Disparities
Fast Facts
Racial and ethnic minority veterans made up about 22% of the total veteran population of 18.6 million in 2016, according to VA.
Mirroring trends seen across the United States, VA has identified worse health care outcomes for some diseases among racial and ethnic minority veterans. For example, VA reported lower survival rates for African American veterans with cancer and cardiovascular-related illnesses than for other minority and white veterans.
We reviewed VA efforts to address these disparities. Among other things, we recommended VA ensure that any plans to address the issue include measures of progress and clear lines of accountability.

Department of Veteran Affairs Headquarters sign
Highlights
What GAO Found
The Department of Veterans Affairs (VA) has taken steps to reduce disparities in health care outcomes linked to race and ethnicity, but lacks mechanisms to measure progress and ensure accountability for results. In 2012, VA established the Office of Health Equity to identify and address health care outcome disparities and to develop an action plan to achieve health equity. This office issued an action plan in 2014 that identified activities to make improvements in five focus areas, such as increasing awareness of the significance of disparities and strengthening leadership for addressing them. However, GAO found that the extent of VA's progress in implementing the action plan and advancing health equity is unknown because the action plan lacked performance measures and clear lines of accountability for specific offices. For example, although VA's action plan included a list of “success criteria” for each of the five focus areas, these criteria were not measurable, and were not linked to specific activities or to offices responsible for implementation.
VA funds research efforts that have identified disparities in health care outcomes involving minority veterans, but rely on data that VA officials and researchers noted have weaknesses in completeness and accuracy. One concern is that race and ethnicity information can be labeled incorrectly in VA patients' electronic health records as ”self-reported”, a highly reliable method of collection, when data were actually collected based on the less reliable method of VA staff observation. Other reported concerns include missing values on patients' race and conflicting race and ethnicity information. VA researchers told GAO they account for some of these concerns by using data from other sources, such as Medicare, but such work-arounds are time intensive. Further, VA officials reported that data weaknesses limit their ability to identify and address disparities in health care outcomes in their medical centers. Despite recognizing weaknesses related to the quality of race and ethnicity data, VA has not implemented corrective actions to address them. Without doing so, VA medical center officials cannot readily identify and address disparities in health care outcomes by race and ethnicity.
Concerns Raised by Department of Veterans Affairs (VA) Officials about the Completeness and Accuracy of VA Race and Ethnicity Data
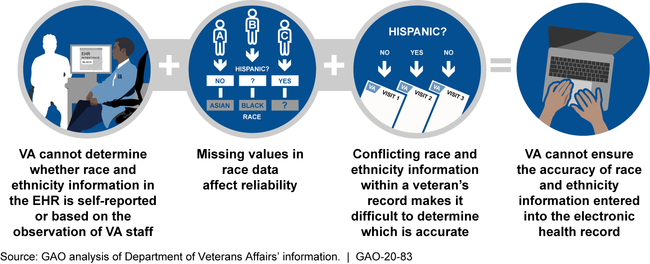
Note: Concerns about the completeness and accuracy of race and ethnicity information were raised by officials from VA's Office of Health Equity, Veterans Experience Office, and Health Services Research & Development.
Why GAO Did This Study
According to VA, in 2016, racial and ethnic minority veterans represented about 22 percent of the total veteran population of 18.6 million. VA projects racial and ethnic minority veterans will make up 36 percent of its total veteran population by 2040. VA has identified racial and ethnic disparities in its health care outcomes, mirroring trends seen across the United States.
House Report 115-188 included a provision for GAO to review whether VHA provides quality, equitable care for minority veterans. GAO's report examines, among other issues, (1) the extent to which VA has taken steps to advance health equity for racial and ethnic minority veterans, and (2) VA's efforts to use race and ethnicity data to identify and address disparities in health care outcomes involving minority veterans. GAO reviewed relevant documents, such as strategic and operational plans and peer-reviewed research studies; assessed VA's health equity action plan against criteria identified in GAO's body of work on effectively managing performance; and interviewed VA officials familiar with VA's health equity efforts, as well as race and ethnicity data.
Recommendations
GAO is making two recommendations to VA to (1) ensure that any health equity action plan includes performance measures to assess progress, and clear lines of accountability designating responsibility to specific offices, and (2) conduct an assessment to determine how to address weaknesses identified with the completeness and accuracy of race and ethnicity data in the electronic health record, and implement corrective actions as necessary. VA agreed with GAO's recommendations.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Office of the Under Secretary for Health | The Under Secretary for Health should ensure that any action plan for achieving health equity includes key elements for successful implementation by consistently applying criteria identified in GAO's past work on effectively managing performance, including developing performance measures to assess progress and creating clear lines of accountability by designating specific offices or officials with responsibility for coordinating efforts to implement actions and committing resources necessary for achieving its goals and objectives. (Recommendation 1) |
VA concurred with our recommendation. In November 2019, VA reported that it planned to develop annual health equity operational plans that include performance measures, clear lines of accountability, and commitment of necessary resources for achieving VHA's health equity goals. In July 2022, OHE shared with GAO its FY 2022 Operational Plan; this version included key elements needed to achieve successful implementation.
|
| Office of the Secretary for VA | To ensure the availability of information on health care outcomes by race and ethnicity throughout the VA health care system, the Secretary of Veterans Affairs should conduct an assessment to determine the completeness and accuracy of race and ethnicity data captured in VA's electronic health record, and implement corrective actions as necessary to resolve any identified deficiencies. (Recommendation 2) |
VA concurred with our recommendation. VA provided documentation of its January 2022 study that assessed the completeness and accuracy of the calendar year 2021 race and ethnicity data in VA's electronic health records. The study noted that that the completeness of race and ethnicity data has improved over time and the 2021 data were complete for 92 percent of veterans receiving care at VA. The study also noted that accuracy was strong for ethnicity data (Hispanic or not Hispanic). Similarly, VA reported that the accuracy of race data for Asian, black/African American and white veterans, which account for over 95 percent of the veteran population, according to VHA Office of Health Equity (OHE). VA has provided technical assistance and disseminated best practices on improving completeness of race and ethnicity data to nine VA medical centers that VA identified as outliers in terms of data completeness; VA continues to monitor these nine VA medical centers for improvements. VA's efforts to hire full time staff whose efforts will focus on providing technical assistance to medical facilities widely demonstrates the department's long term commitment to ensuring that this these data continue to be complete and accurate. Based on the evidence VA provided, GAO has closed this recommendation as implemented.
|
