Racial Disparities in Health Care and the Role of Government
Over the past several years, GAO has been asked to examine various racial inequalities in public programs and we have made recommendations to find and address them.
Today’s WatchBlog looks at disparities in health care.
Maternal Mortality
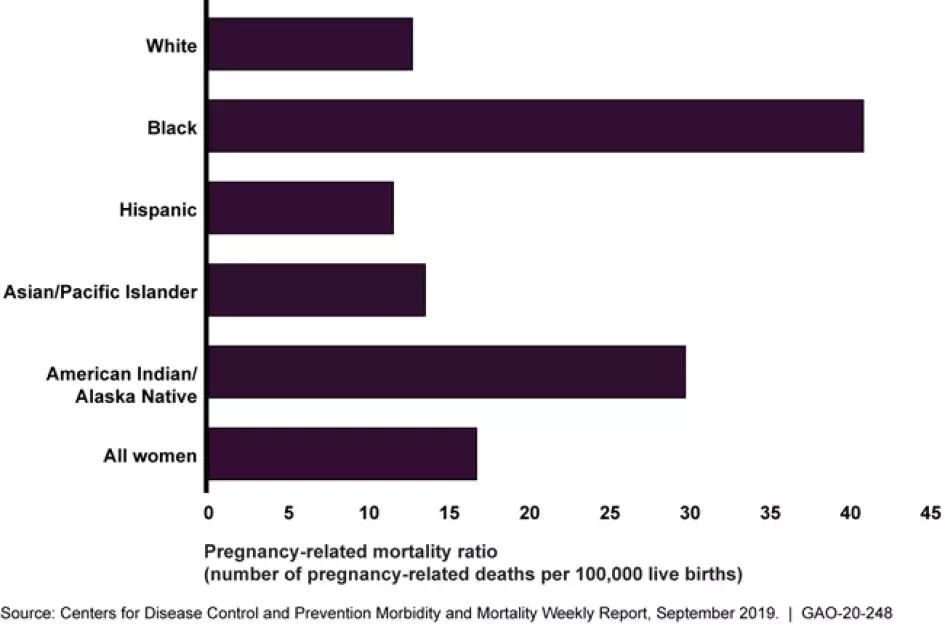
Our work has found disparities between White and minority groups’ health care outcomes and access to health care. For example, in March, we reported that non-Hispanic Black mothers were more than 3 times more likely to die during child birth than non-Hispanic White mothers. Contributing factors that are considered when reviewing these deaths include systemic factors, such as access to care, as well as patient and provider factors, such as lack of knowledge of warning signs, or missing or delayed diagnoses.
Figure: Pregnancy-Related Deaths per 100,000 Live Births by Ethnic/Racial Group, 2007-2016
Veterans’ Health
We have also reported on disparities in health care outcomes for our nation’s Black veterans. In December 2019, we reported that the Veterans Administration has identified worse health care outcomes among racial and ethnic minority veterans, mirroring trends across the United States. In 2011, the VA found outcomes for controlling blood pressure, blood glucose, and cholesterol levels were significantly worse for Black veterans than they were for White veterans. In 2019, the VA reported evidence of disparities in health care outcomes within VA medical centers in the form of lower survival rates Black veterans with cancer and cardiovascular-related illnesses compared with other minority veterans and White veterans. Our report did not look at differences in medical treatments and how they might impact outcomes. However, in both our reports on maternal and veteran outcomes, we recommended that federal agencies improve their collection and use of data to help inform decisions that could improve health care outcomes for Black and other patients.
Environmental Health Factors
In September 2019, we found that low-income and minority communities across the country were disproportionately exposed to facilities that emit harmful air pollution (e.g., industrial or waste disposal facilities). For example, the predominantly minority and low-income community of West Oakland, California, is surrounded by 3 interstate freeways and abuts a major port that brings up to 3,000 trucks to the area each day. A study conducted in 2008 found that West Oakland residents were exposed to diesel pollutants at levels almost 3 times higher than average background levels in the surrounding area.
In addition to harmful air pollution, other environmental justice issues include unsafe drinking water, proximity to chemical facilities, and risks from climate change and natural disasters. Federal agencies have been making efforts to identify and address environmental justice issues for more than 25 years. However, we have made a number of recommendations to improve this effort, including 24 recommendations in our September 2019 report, which have not been implemented by agencies.
For more about our work on Health Care policy and trends, check out our key issues pages.
Comments on GAO’s WatchBlog? Contact blog@gao.gov.