Maternal Mortality: Trends in Pregnancy-Related Deaths and Federal Efforts to Reduce Them
Fast Facts
Every year in the U.S., hundreds of women die of complications related to pregnancy and childbirth. Mortality varies by race/ethnic group. For example, non-Hispanic black women are more than 3 times as likely to die as non-Hispanic white women, according to the CDC.
This report describes, among other things, Health and Human Services’ ongoing efforts to prevent these deaths. For example, it funds committees in 25 states that comprehensively review maternal mortality and identify ways to prevent it. Officials in the 5 states where we conducted interviews said they were beginning or continuing to address racial/ethnic health differences.
Pregnancy-Related Deaths per 100,000 Live Births by Ethnic/Racial Group, 2007-2016
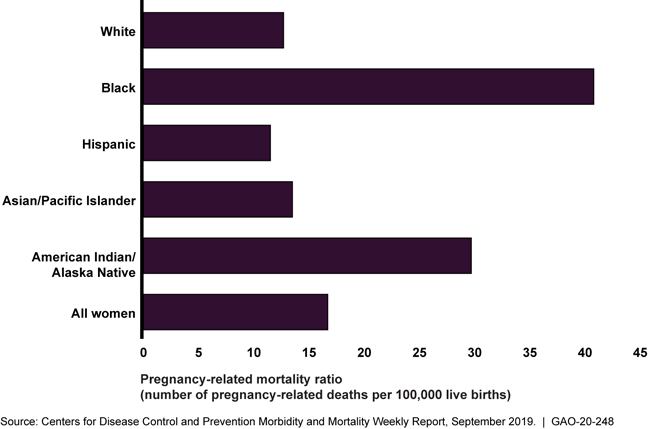
Bar chart showing between 40 and 45 deaths per 100 by ethnic/racial group
Highlights
Why GAO Did This Study
Every year in the United States, hundreds of women die of complications related to pregnancy and childbirth. According to CDC data, racial/ethnic disparities exist with regard to these deaths. For example, non-Hispanic black women were more than three times as likely to die as non-Hispanic white women, and non-Hispanic American Indian/Alaska Native women were more than two times as likely to die as non-Hispanic white women.
GAO was asked to review issues related to maternal mortality in the United States. In this report, GAO describes, among other things, (1) trends in pregnancy-related deaths in the United States, including trends in causes and timing of these deaths, and (2) HHS funding efforts focused on reducing pregnancy-related deaths.
GAO reviewed documentation about HHS's surveillance efforts related to pregnancy-related deaths; and analyzed CDC data on leading causes of pregnancy-related deaths from 2007 through 2016 (the most recent 10-year period available at the time of GAO's review). GAO also reviewed documentation and interviewed HHS and state public health officials in five selected states about HHS's funding efforts aimed at reducing pregnancy-related deaths, including select efforts used in these states. GAO selected these states primarily based on their geographic diversity and their implementation of select efforts to address maternal mortality. GAO provided a draft of this report to HHS. HHS provided technical comments, which GAO incorporated as appropriate.
What GAO Found
GAO's analysis of the Centers for Disease Control and Prevention's (CDC) Pregnancy Mortality Surveillance System data shows that from 2007 through 2016, over 6,700 women died of causes related to or aggravated by their pregnancy—either while pregnant or within 1 year of the end of pregnancy. While CDC data show an overall increase in the pregnancy-related mortality ratio in the United States during this time frame, the annual ratio fluctuated. Cardiovascular conditions, infection, and hemorrhage were the leading causes of pregnancy-related deaths, and comprised about 50 percent of all pregnancy-related deaths from 2007 through 2016. In addition, CDC data show that the leading causes of pregnancy-related deaths differed by racial ethnic groups. (See figures.)
Figure: Leading Causes of Pregnancy-Related Deaths by Select Racial/Ethnic Groups, 2007-2016
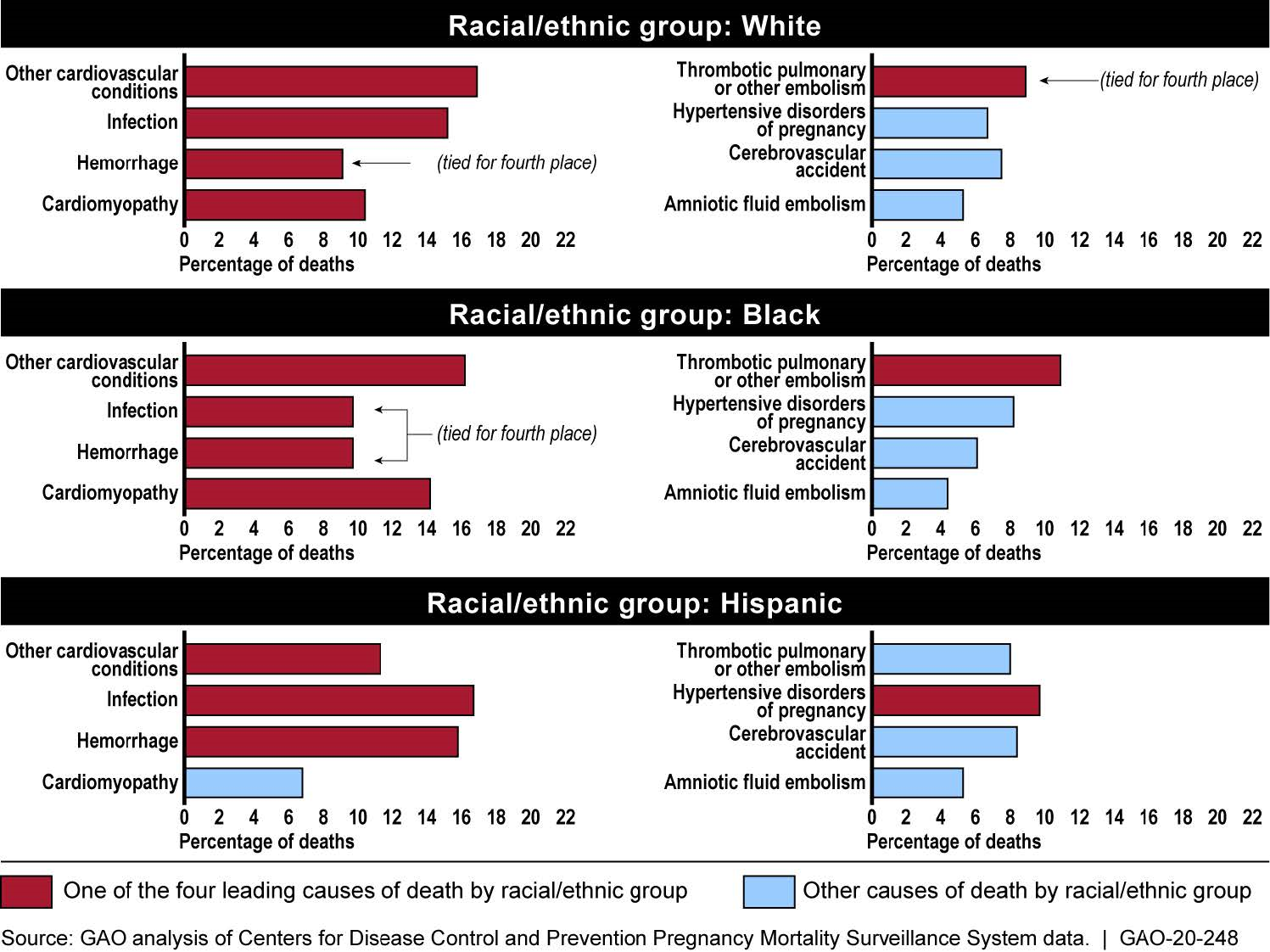
Notes: “Other cardiovascular conditions” includes conditions not reported separately as cardiomyopathy—when the normal muscle in the heart thicken, stiffen, thin out, or fill with substances the body produces that do not belong in the muscle, or cerebrovascular accidents—known as stroke.
Pregnancy-related death, as defined in statute, is the death of a woman while pregnant or within 1 year of the end of a pregnancy— regardless of the outcome, duration or site of the pregnancy—from any cause related to or aggravated by the pregnancy or its management, but not from accidental or incidental causes. 42 U.S.C. § 247b-12(e)(3).
White and black women were non-Hispanic. Hispanic women might be of any race.
Figure: Pregnancy-Related Deaths per 100,000 Live Births by Racial/Ethnic Group, 2007-2016
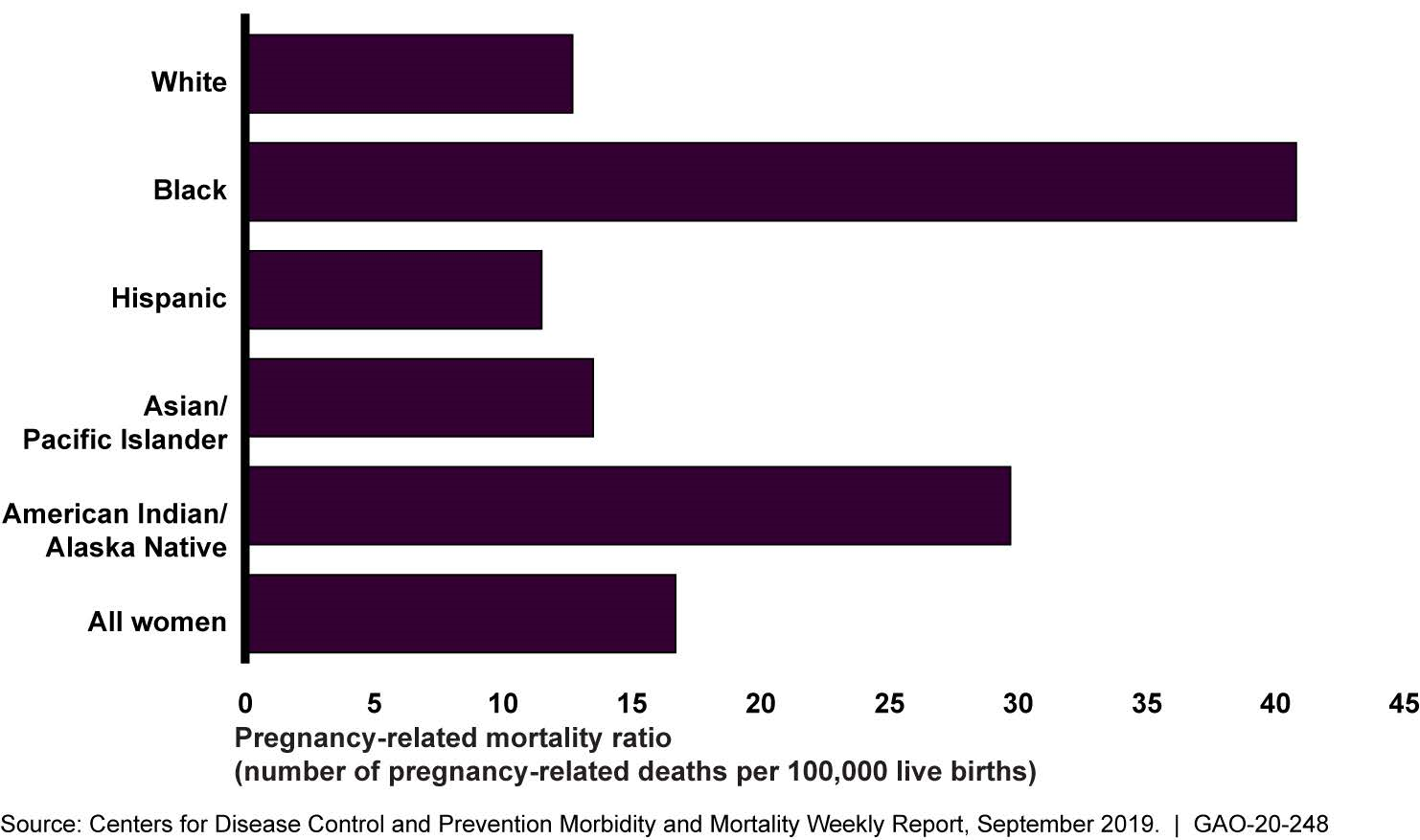
Notes: White, black, American Indian/Alaska Native and Asian/Pacific Islander women were non-Hispanic. Hispanic women might be of any race.
The Department of Health and Human Services has 13 ongoing efforts aimed at reducing pregnancy-related deaths. The following are key examples of these:
- Supporting Maternal Mortality Review Committees Cooperative Agreements. According to CDC officials, in September 2019, CDC awarded 5-year cooperative agreements to 24 recipients covering 25 states with amounts ranging from $150,000 to over $550,000 in the first year, totaling about $8.4 million. Under these agreements, CDC is providing funding to state agencies and organizations that coordinate and manage Maternal Mortality Review Committees. The committees are responsible for comprehensively reviewing deaths to identify prevention opportunities.
- Maternal and Child Health (MCH) Services Block Grant Program.The Health Resources and Services Administration provides funding through this program to 59 states and jurisdictions to improve maternal and child health. In fiscal year 2017, total expenditures for services for pregnant women from all sources—federal funds, as well as state, local, program income, and other funds—was about $300 million. According to agency officials, many recipients reported using their block grant funding to help support or complement other federal initiatives, such as their review committee, quality collaborative, and use of maternal safety bundles.
According to officials GAO interviewed in five selected states, they use these efforts and others collectively to address pregnancy-related deaths. For example, according to officials in one state, they implemented an obstetric hemorrhage maternal safety bundle in 2018 based on the state's Maternal Mortality Review Committee finding that hemorrhage was a leading cause of pregnancy-related deaths in the state. According to officials, the state's Maternal Mortality Review Committee was funded primarily through the MCH Services Block Grant.
All five states also mentioned beginning or continuing to address racial/ethnic or other health disparities with block grant funding, through their Maternal Mortality Review Committees, or other efforts. For example, officials in one state said they use block grant funding to support their Black Infant Health Program, which helps address maternal morbidity and mortality of black mothers in the late maternal period. Additionally, two of the HHS funding efforts awarded in fiscal year 2019 have outcomes related to decreasing racial and ethnic disparities in maternal mortality: the Alliance for Innovation on Maternal Health Community Care Initiative and the State Maternal Health Innovation Program.
For more information, contact Mary Denigan-Macauley at (202) 512-7114 or deniganmacauleym@gao.gov.
