Science & Tech Spotlight: Long COVID
Fast Facts
How many people in the U.S. have developed "long COVID"?
It could be in the range of 7.7–23 million, some estimates say.
We discuss what is and isn't known about long COVID—new, returning, or ongoing health problems 4 or more weeks after an initial case of COVID-19. For example, some people with the condition experience chronic fatigue and have to stop working, which can affect their income and health insurance. But other economic effects are still unclear.
The federal government is taking steps to fund more research and help affected people. We describe challenges it could encounter and provide questions for policymakers to consider.
Highlights
Why This Matters
Long COVID has potentially affected up to 23 million Americans, pushing an estimated 1 million people out of work. The full magnitude of health and economic effects is unknown but is expected to be significant. The causes of long COVID are not fully understood, complicating diagnosis and treatment. The condition raises policy questions, such as how best to support patients.
The Science
What is it? Long COVID, according to the Centers for Disease Control and Prevention (CDC), is the occurrence of new, returning, or ongoing health problems 4 or more weeks after an initial infection with SARS-CoV-2, the virus that causes COVID-19. It is also known by other names, including post-acute COVID, post-COVID conditions, and chronic COVID.
Symptoms of long COVID vary from person to person. They may include fatigue, cognitive impairment (or "brain fog"), muscle or joint pain, shortness of breath, heart palpitations, sleep difficulties, and mood changes (see fig. 1). Long COVID can affect multiple organ systems and cause tissue damage.
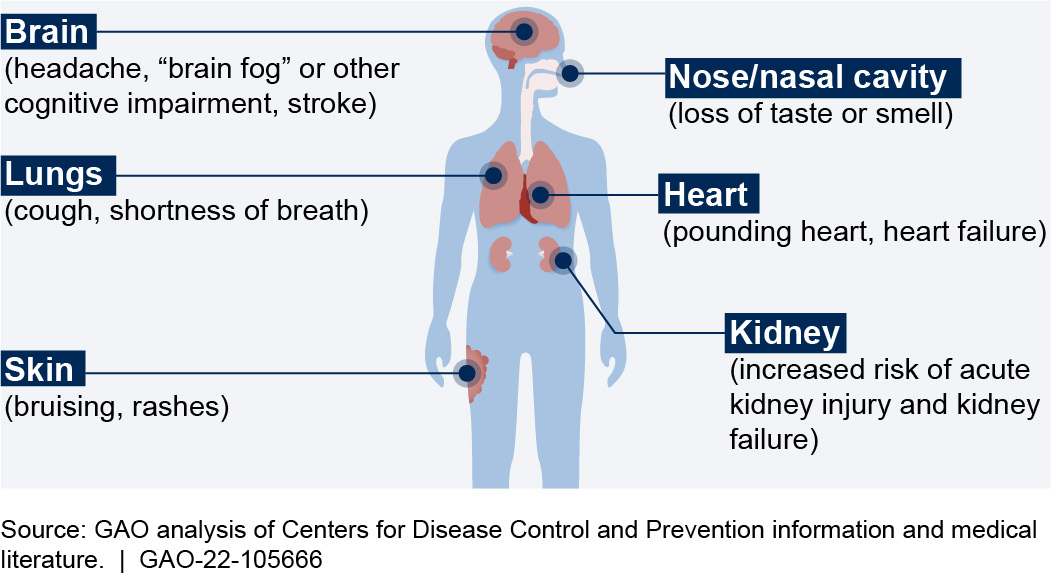
Figure 1. Some reported symptoms of long COVID.
Long COVID is a post-viral syndrome. Post-viral syndromes are well documented for a range of infections. For example, one study found that more than 27 percent of survivors from another coronavirus, severe acute respiratory syndrome (SARS), had chronic fatigue syndrome 4 years after their initial infection.
What is known? Long COVID can have serious impacts. Some individuals have reported a need to adjust their work hours or stop working altogether due to chronic fatigue or cognitive impairment. One study of nearly 4,000 long COVID patients found that 45 percent reduced their work hours. For some, the change in job status can affect health insurance, which can further complicate treatment options. Individuals have also said their symptoms interfere with childcare, exercise, and social activities. This disruption of their daily lives can cause mental health issues. Another study used the electronic health records of more than 200,000 COVID-19 survivors and found that within 6 months following initial infection, one-third experienced neurological or psychological symptoms such as anxiety, depression, post-traumatic stress disorder, and psychosis.
What are the knowledge gaps? Researchers do not yet fully understand the risk factors, causes, and effects of long COVID. Risk factors include preexisting conditions, such as type 2 diabetes. Severity of COVID-19 may also be a predictor, although people with mild or asymptomatic infections can also develop the syndrome. Whether vaccination for COVID-19 reduces an infected person's risk of developing long COVID is unclear. Some studies have suggested that vaccination reduces risk by up to 50 percent, while others have found no reduction in risk.
Researchers have identified several possible causes of long COVID and have suggested that causes may vary from person to person (see fig. 2). For some, COVID-19 may cause the body to produce an antibody that mimics SARS-CoV-2 and triggers an autoimmune response in which the immune system attacks its own antibodies. For others, SARS-CoV-2 virus may persist in the body and cause symptoms. Another possible cause is organ damage from COVID-19. Research also suggests that microclots may form in blood vessels, blocking blood flow and causing tissue damage. And COVID-19 may disrupt the immune system and reactivate other previously contracted viruses, such as Epstein-Barr.
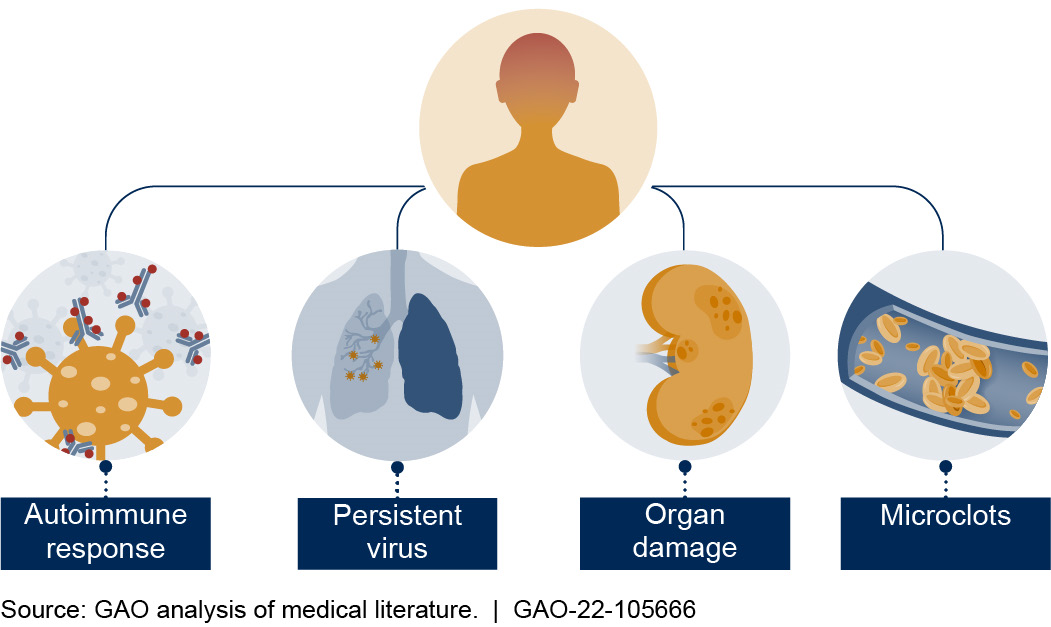
Figure 2. Some possible causes of long COVID as suggested by researchers.
Researchers are working to develop methods to reliably diagnose and treat long COVID. Health care providers may use COVID-19 antibody tests in an attempt to confirm previous infection, then rule out other conditions that may cause similar symptoms. Treatment strategies are based on patients' specific symptoms and may include existing therapeutics, such as steroids or anti-inflammatory medication. Trials are underway to test new therapeutics for long COVID patients.
The broader public health, social, and economic effects of long COVID are unclear. Studies in the U.S. estimate that 10 to 30 percent of COVID-19 survivors develop long COVID. If so, 7.7 million to 23 million people in the U.S. may have developed long COVID as of February 2022. In January 2022, the Brookings Institution conducted a meta-analysis to suggest that long COVID may be responsible for over 1 million workers being out of the labor force at any given time.
What is being done? The federal government is taking steps to fund additional long COVID research. For example, the National Institutes of Health launched the $1.15 billion Researching COVID to Enhance Recovery (RECOVER) Initiative, which combines data across more than 200 research sites. The initiative is using electronic health records to group common characteristics of tens of thousands of volunteers to better identify risk factors and causes of long COVID. Similarly, the CDC has contracted for a study in which patients voluntarily share their health data through a cloud-based personal health platform.
The federal government has also taken steps to support long COVID patients. For example, the Departments of Justice and Health and Human Services (HHS) issued guidance stating that the condition can be a disability under the Americans with Disabilities Act of 1990. Some long COVID patients may qualify for Social Security Disability Insurance (SSDI) if they meet certain requirements. The CDC has developed long COVID guidance for health care providers and the public. Another HHS agency, the Administration for Community Living, published a guide to community-based resources to help connect affected people to services like transportation and personal care attendants.
Non-governmental experts and organizations are also addressing long COVID. For example, the National Academies of Sciences, Engineering, and Medicine will hold a public workshop in March 2022 to discuss several long COVID topics, including effects on children, mental health, and labor, as well as the effects of vaccines. In addition, researchers are applying machine learning to patient data to identify symptoms, and many hospital systems are forming specialized clinics to treat and support patients.
Challenges
- Research. Researchers have struggled to identify some causes of other post-viral and bacterial syndromes, such as chronic fatigue syndrome and post-treatment Lyme disease syndrome. They may face similar challenges with long COVID.
- Diagnosis and treatment. Some patients report difficulty obtaining a long COVID diagnosis, which complicates efforts to get support, such as disability assistance and clinical care. Patients experiencing several symptoms may need to consult with multiple specialists. In addition, without consistent diagnoses, national data will not be adequate to track and respond to the condition.
- Economic effects. People with long COVID might leave the workforce, causing them to lose wages and employer-based health insurance. This could affect the broader U.S. economy through decreased labor participation and an increased need for use of SSDI or other publically subsidized insurance.
Policy Context and Questions
- How can policymakers support research initiatives and improve data collection on long COVID, including to identify trends?
- What programs can policymakers leverage or develop to provide support to those with long COVID?
- How can policymakers guide health care workers and inform the public about long COVID?
- What steps can policymakers take to address potential economic effects of long COVID?
For more information, contact Karen Howard at 202-512-6888 or HowardK@gao.gov.
