COVID-19 in Nursing Homes: CMS Needs to Continue to Strengthen Oversight of Infection Prevention and Control
Fast Facts
The COVID-19 pandemic caused severe illness and death in many nursing homes across the U.S. We also found that some indicators of resident mental and physical health worsened during the pandemic.
The pandemic also highlighted long-standing problems with infection prevention and control in nursing homes. Before the pandemic, the Centers for Medicare & Medicaid Services began requiring nursing homes to designate an infection preventionist on staff. The preventionist is responsible for the home's infection prevention and control program—playing a critical role during the pandemic. We found that the agency could strengthen the preventionists' role, including by collecting preventionist staffing data.
Our recommendations address this issue and more.

Highlights
What GAO Found
The Centers for Medicare & Medicaid Services (CMS) is responsible for ensuring that nursing homes meet federal standards. CMS enters into agreements with state survey agencies to conduct surveys and investigations of the state's nursing homes. The Centers for Disease Control and Prevention (CDC) issues guidance, operates surveillance systems, and provides technical assistance to support infection prevention and control in nursing homes.
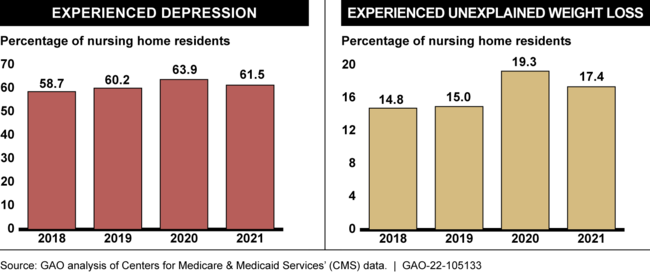
GAO analysis of CMS data reported by nursing homes shows that seven of the eight key indicators of nursing home resident mental and physical health worsened at least slightly the first year of the pandemic (2020), compared to the years prior to the pandemic. See the figure below for examples of two outcomes we reviewed.
Percentage of Residents Who Experienced Depression and Unexplained Weight Loss, by Year
CMS and CDC took actions on infection prevention and control prior to and during the COVID-19 pandemic. For example, prior to the pandemic, CMS required nursing homes to designate an infection preventionist on staff. This person is a trained employee responsible for the home's infection prevention and control program and was crucial to nursing homes during the pandemic. CMS also made changes in how nursing homes were surveyed during the pandemic. However, GAO found areas where CMS could take additional actions, including:
- Strengthening oversight of the infection preventionist role. GAO identified ways CMS could strengthen oversight of the infection preventionist role, such as by establishing minimum training standards. CMS could also collect infection preventionist staffing data and use it to determine whether the current infection preventionist staffing requirement is sufficient.
- Strengthening infection prevention and control guidance. GAO identified how CMS could strengthen this guidance by providing information to help surveyors assess the scope and severity of infection prevention and control deficiencies they identify. For example, CMS could add COVID-19-relevant examples for scope and severity classifications to its State Operations Manual—the key guidance state survey agencies use for conducting nursing home surveys.
Why GAO Did This Study
Implementing proper infection prevention and control practices can be critical for preventing the spread of infectious diseases. Infection prevention and control has been a long-standing concern in the nation's more than 15,000 nursing homes—one that the COVID-19 pandemic has brought into sharper focus. Some infection prevention and control practices in nursing homes, such as social isolation, may negatively affect resident mental and physical health.
The CARES Act directs GAO to monitor the federal pandemic response. GAO was also asked to review federal oversight of nursing homes in light of the pandemic. Among other objectives, this report: (1) describes what data reveal about any changes in resident health before and during the pandemic and (2) examines infection prevention and control actions CMS and CDC have taken in nursing homes before and during the pandemic.
GAO (1) reviewed CMS and CDC documents, (2) analyzed CMS resident health data from 2018 through 2021, and (3) interviewed CMS, CDC, state survey agency, and nursing home officials in a non-generalizable sample of eight states selected for variation in factors such as geographic location.
Recommendations
GAO is making three recommendations to CMS related to the role of the infection preventionist and clarifying infection prevention and control guidance. HHS agreed with our first recommendation, but neither agreed nor disagreed with our other two recommendations.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Centers for Medicare & Medicaid Services | The Administrator of CMS should establish minimum infection preventionist training standards. (Recommendation 1) |
HHS concurred with this recommendation. In March 2023, HHS said that CMS is continuing its comprehensive review of nursing home infection control, which has a targeted completion date of December 2023. In April 2024, CMS said that it has reviewed the existing requirements for infection preventionist training in nursing homes and the agency believes the requirements are appropriate and effective. In March 2025, CMS said it does not prescribe the exact amount or type of infection preventionist training that facilities must provide to their staff, but the agency expects nursing homes to provide the training needed to ensure staff have the appropriate skills to do their job. In January 2026, CMS said it intentionally does not prescribe a single, standardized training program or a fixed number of training hours, which allows facilities to tailor infection preventionist training to their specific setting. We maintain that establishing minimum infection preventionist training standards remains important.
|
| Centers for Medicare & Medicaid Services | The Administrator of CMS should collect infection preventionist staffing data and use these data to determine whether the current infection preventionist staffing requirement is sufficient. (Recommendation 2) |
HHS did not state whether it agreed or disagreed with this recommendation. In March 2025, HHS said that CMS will evaluate the feasibility of collecting this information and take appropriate actions based on its evaluation. The target date for completing this action is January 2026.
|
| Centers for Medicare & Medicaid Services | The Administrator of CMS should provide additional guidance in the State Operations Manual on making scope and severity determinations for IPC-related deficiencies. (Recommendation 3) |
HHS did not state whether it agreed or disagreed with this recommendation. In November 2024, CMS issued an advance copy of planned revisions to the State Operations Manual addressing the scope and severity determinations for Infection Prevention and Control (IPC)-related deficiencies. These revisions, which went into effect in April 2025, clarify guidance for state survey agencies by providing examples for IPC deficiencies specific to COVID-19 and other respiratory diseases, therefore addressing our recommendation.
|
