VA Community Living Centers: Opportunities Exist to Strengthen Oversight of Quality of Care
Fast Facts
VA provides care to about 9,000 veterans in 134 VA-operated nursing homes, called "community living centers." For oversight, VA conducts unannounced inspections and tracks quality measures (such as the percentage of residents with a fall) and nurse staffing levels.
Performance generally improved from FY 2015-FY 2019. For example, inspections found fewer practices that caused actual harm. But deficiencies didn't consistently trend downward and individual centers showed mixed results.
Our 3 recommendations seek to improve VA's oversight by clarifying which quality standards the centers should meet and gathering additional data on care quality.

Highlights
What GAO Found
The Department of Veterans Affairs (VA) provides care to around 9,000 veterans each day in its 134 VA-operated nursing homes, called community living centers (CLC). VA has based its CLC oversight and quality improvement efforts on data from three sources: results of unannounced inspections, scores on clinical quality measures (such as residents with recent falls), and nurse staffing levels. GAO analyzed these data and found that, nationally, CLC performance generally improved on inspections and clinical quality measures, and staffing levels increased from fiscal years 2015 through 2019, the most recent complete data available. Results varied among individual CLCs (see figure).
Community Living Center (CLC) Performance on Unannounced Inspections, Fiscal Years (FY) 2015 – 2019
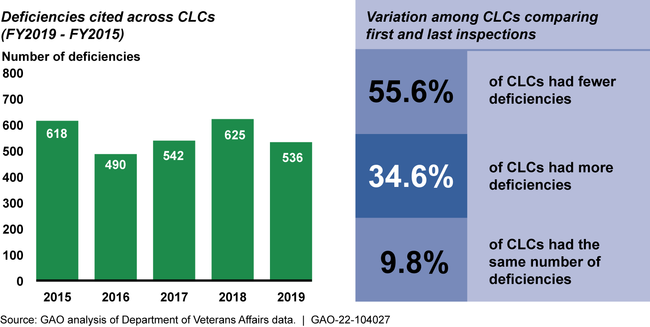
GAO found opportunities to strengthen VA's oversight related to VA's policies and the availability of other key data. For example:
VA's CLC policies do not identify applicable quality standards.
- According to VA officials, during unannounced inspections, CLCs are evaluated against the same quality standards as community nursing homes, except when superseded by VA policy. However, as of September 2021, VA's CLC-related policies and training documentation did not identify the instances when VA policies apply instead. VA officials stated the agency is currently revising its CLC-related policies, but the revision will not address these gaps.VA could help ensure CLC providers and staff adhere to the appropriate standards by addressing these gaps.
VA has not surveyed current residents about their CLC experience.
- Patient experience surveys are key tools for measuring quality and would help VA meet its strategic goal of providing residents with a voice in their care. Current CLC residents are not included in VA's existing patient experience surveys. Although VA officials reported plans to develop such a survey specifically for CLC residents, it is not currently a priority. A survey for CLC residents would help VA identify quality of care issues across CLCs.
Why GAO Did This Study
VA is responsible for overseeing the quality of care provided in its CLCs, such as through unannounced inspections that identify deficiencies when CLCs do not meet quality standards. However, recent reports have raised questions about substandard treatment and conditions at certain CLCs, as well as about the transparency of VA data on CLC quality.
GAO was asked to examine VA data on CLC quality and how the data are used to oversee CLCs. In this report, GAO describes what VA data reveal about quality at the CLCs and assesses VA's oversight of CLCs and how, if at all, it could be strengthened, among other issues.
To perform this work, GAO reviewed VA policies, analyzed the most recent 5 years of complete data on CLC quality at the time of its review, and interviewed VA officials. GAO also selected six VA CLCs based on factors such as CLC performance on VA's quality ratings website and location. For each, GAO interviewed CLC officials and officials from corresponding VA regional offices.
Recommendations
GAO is making three recommendations, including for VA to update its policy and training documentation to identify the quality standards CLCs are required to follow and to prioritize development of a standard survey on CLC resident experiences. VA agreed with GAO's recommendations.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Department of Veterans Affairs | The Department of Veterans Affairs Under Secretary of Health should update policy and training to identify the quality standards CLCs are required to follow in the CMS State Operations Manual and specify when VA policy standards supersede CMS quality standards. (Recommendation 1) |
VA concurred with this recommendation. In April 2022, VA said that it is reviewing CLC policies related to quality standards within the CLCs and the CMS State Operations Manual. In April 2023, VA provided a crosswalk it developed that maps the applicable CMS State Operations Manual regulations and policy authorities superseded by VA policies and directives. This crosswalk was distributed to all CLCs and a training was held for staff. However, VA's policy related to quality standards for CLCs continues to reflect inaccurate standards. In October 2023, VA released VHA Directive 1142, which it describes as a "one-stop shop" to define CLC processes, procedures, and practices. They also rescinded several older CLC related directives and handbooks. This new directive and the crosswalk reflect the quality standards CLCs are expected to meet.
|
| Department of Veterans Affairs | The Department of Veterans Affairs Under Secretary of Health should ensure that NCPS collects reliable patient safety data for CLCs by standardizing how VAMCs record the location of patient safety events, including those that occurred at the CLC, in JPSR and subsequently share the aggregate data with CLCs. (Recommendation 2) |
VA concurred with this recommendation. In April 2022, VA stated that its National Center for Patient Safety was in the process of collecting and analyzing information to create a CLC naming convention. In April 2023, VA stated that the National Center for Patient Safety made more than 50 naming convention changes as a result of its work to identify CLCs that were previously not identified in JPSR and that this work was completed by its software vendor from September 2022 to January 2023. The National Center for Patient Safety updated the JPSR Business Rules in December 2022 to add the requirement that patient safety events occurring CLCs must be identified using the new naming convention. This should allow VA to reliably identify which patient safety events occurred within CLCs. The National Center for Patient Safety and Geriatrics and Extended Care offices collaborated on developing a report of aggregated patient safety information related to CLCs, which they now share quarterly with CLCs.
|
| Department of Veterans Affairs | The Department of Veterans Affairs Under Secretary of Health should prioritize the development and implementation of a standardized survey to obtain data on current resident experiences of the quality of care at the CLCs. (Recommendation 3) |
VA concurred with this recommendation. In April 2022, VA stated that its Geriatrics and Extended Care Office is partnering with the VA Veterans Experience Office to implement a CLC satisfaction survey. In April 2023, VA stated that its Veterans Experience Office had completed four onsite visits, the research portion of the survey creation, and provided an overview of its findings to the Geriatrics and Extended Care Office. VA provided documentation indicating that VA completed the design phase of the survey and began implementing the survey at four pilot CLCs in June 2023. VA plans to implement the survey at all CLCs by October 2023.
|
