Veterans Health Care: Actions Needed to Improve the Foreign Medical Program
Fast Facts
Veterans with service-related disabilities living or traveling abroad may use health care benefits through the Department of Veterans Affairs' Foreign Medical Program.
The program has had trouble reimbursing some veterans and doctors. For example, despite a federal law calling for electronic payments, the program sends paper checks—sometimes resulting in lost or delayed payments. VA began transitioning to an electronic payment system, but it's unclear when it will be complete.
VA also authorized hiring additional staff to speed up the reimbursement process, but many of those positions remain vacant.
Our recommendations address this, and more.

Highlights
What GAO Found
The Department of Veterans Affairs (VA) is responsible for providing benefits to veterans. Within VA, the Veterans Health Administration (VHA) provides health care benefits to eligible veterans with service-connected disabilities living or traveling abroad through its Foreign Medical Program. In fiscal year 2024, VHA data show the program paid $128.3 million in reimbursements to 8,024 veterans or their providers, representing a 263 percent increase in reimbursements since fiscal year 2018. In fiscal year 2024, the program reported processing 37 percent of claims within 45 days; its goal is to process 90 percent within that time.
Foreign Medical Program Reimbursements, Fiscal Years 2018 through 2024
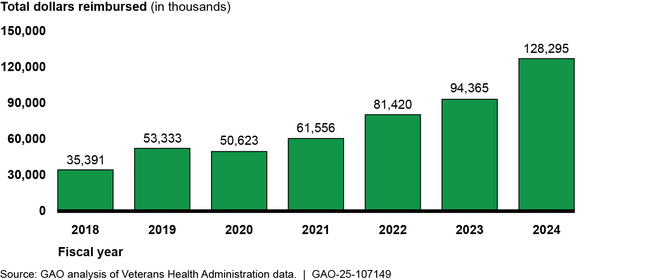
The Foreign Medical Program makes reimbursements using paper checks, despite a federal law generally calling for electronic payments. Reliance on paper checks has resulted in challenges, including delayed or lost checks, according to officials. VA has begun a transition to an electronic payment method, but when or how the transition will occur is unclear. Implementing the new method will help ensure the timeliness and security of reimbursements.
VHA increased its authorized staffing in August 2023 from 25 to 38 positions for the Foreign Medical Program to help meet its timeliness goal. However, 14 positions remained vacant in 2024 due to various reasons, including a VHA zero-growth hiring policy, according to officials. VHA has taken some steps to help with hiring, such as allowing positions to be remote, but has not otherwise identified and evaluated staffing strategies. Evaluating and implementing such strategies could help the program address its staffing challenges and process claims in a timely manner.
VA has not comprehensively assessed fraud risks in the program in line with selected leading practices, despite evidence of potential fraud. This included VA suspending providers in 2024 due to their alleged involvement in a long-term fraud scheme. VHA developed two documents to outline efforts for fraud, waste, and abuse activities within VHA. However, VA has not implemented selected leading practices outlined in GAO's Fraud Risk Framework. These include assigning an entity to lead and regularly assess fraud risks. Implementing such practices will help VA better prevent, detect, and respond to fraud.
Why GAO Did This Study
Thousands of veterans live in or travel to foreign countries each year. For qualifying medical expenses incurred abroad, veterans, or the providers that deliver services, may submit claims to VHA's Foreign Medical Program for reimbursement.
The Consolidated Appropriations Act, 2023, includes a provision for GAO to review the VHA Foreign Medical Program. This report addresses available data on program claims, VHA processes for reimbursing claims, program staffing, and the extent to which fraud risk management activities for the program are consistent with selected leading practices.
GAO reviewed data on claims processed for fiscal years 2018 through 2024 and relevant program policies and documentation; assessed the program's processes against criteria, such as human capital management key practices and GAO's Fraud Risk Framework; and interviewed agency officials, veterans who use the program, and five veterans service organizations. GAO conducted interviews with veterans in person and obtained written responses via email.
Recommendations
GAO is making nine recommendations to VHA, including that it finalize and prioritize implementation of the steps to transition to electronic funds transfers, evaluate and implement strategies to help mitigate staffing challenges, and follow leading practices for addressing the elements for assessing fraud risks. VA concurred with the recommendations and identified steps VHA plans to take to implement them.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, develop and implement a modernization plan for the program's legacy claims processing system, including milestones, a description of the work necessary, and details on the disposition of the legacy system. (Recommendation 1) |
VA concurred with this recommendation. In January 2025, VA stated the Foreign Medical Program claims processing system modernization is part of a larger modernization portfolio plan and that the estimated completion date for the Foreign Medical Program to transition to a new claims processing system is May 2027. In an October 2025 update, VA stated that the Foreign Medical Program is collaborating with VA's Financial Services Center to migrate claims processing to a modernized system by July 2026 as part of a broader claims migration project. VA planned to complete sunsetting the legacy system sunsetting by January 2026; however, the target completion date has been adjusted to July 2026 to allow for completion of IT development work. In a February 2026 update, VA stated Foreign Medical Program claims processing is on track to transition to the new system in July 2026 and testing is projected to start in March 2026. Claims processing in the legacy system will cease at that time. Once we receive more information on VA's modernization plan, we will assess the extent to which these efforts address our recommendation.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, finalize the necessary steps to transition to electronic funds transfers and immediately prioritize their implementation in coordination with the Department of the Treasury, as appropriate. (Recommendation 2) |
VA concurred with this recommendation. In a July 2025 update, VA stated that electronic funds transfers to domestic bank accounts for the Foreign Medical Program went live in mid-April 2025. VA stated that the project has two additional phases that will be developed concurrently but the estimated target date for completion of these phases has shifted from December 2026 to June 2027 due to unforeseen project and system dependencies that require additional time to complete. In an October 2025 update, VA stated that completion of the first phase of the transition to electronic payment has enhanced the timeliness of payments to veterans. VA stated that programming and process development for the second phase of the transition is ongoing and is anticipated to go live after the program transitions its claims processing to a modernized system planned for July 2026. Once we receive more information on VA's actions to implement electronic funds transfers for the program, we will assess the extent to which these efforts address our recommendation.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, evaluate and implement as appropriate strategies to help mitigate staffing challenges that affect the Foreign Medical Program. (Recommendation 3) |
VA concurred with this recommendation. In January 2025, VA stated that the Foreign Medical Program implemented a range of strategies to address staffing challenges, such as cross training department staff to assist with processing claims during overtime hours and allocating a budget for voluntary overtime. In a July 2025 update, VA stated that per a hiring freeze, VHA is reviewing staffing for its programs, and the Foreign Medical Program is exploring technological solutions and automations to improve efficiencies. VA extended the target completion date to December 2025 to accommodate a staffing review and the exploration of technological solutions. In an October 2025 update, VA stated that the federal hiring freeze remains in effect; however, the program submitted an exemption request in May 2025 to hire additional claims examiners. VA stated the program is developing technology-based solutions, such as automated checks for duplicate claim submissions and auto-adjudication rules in its modernized claims processing system. The expected delivery date for those updates and for VA to address the recommendation is August 2026. In a February 2026 update, VA stated that to improve claim processing timeliness and to mitigate ongoing staffing challenges, the Foreign Medical Program is maximizing the use of voluntary staff overtime and cross departmental staffing, developing technology-based solutions, refining internal processes for efficiency, and using a pool of 25 Office of Integrated Veteran Care volunteers to process claims. VA also stated that in January 2026, a request for a temporary 120-day promotional detail hiring request was initiated for all 16 vacant claims examiner positions. Once we receive more information on VA's review of staffing for the program, we will assess the extent to which these efforts address our recommendation.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, designate a dedicated entity for managing the process of assessing fraud risks to the program, consistent with leading practices. This entity should have, among other things, clearly defined and documented responsibilities, and authority for managing fraud risk assessment for the program. (Recommendation 4) |
VA concurred with this recommendation. In a February 2026 update, VA provided an updated standard operating procedure document that designates an entity for managing the process of assessing fraud risks in the program. The standard operating procedure clearly defined and documented responsibilities for the entity and provided it with authority for managing assessment of fraud risk in the program. We consider this recommendation implemented.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, regularly identify inherent fraud risks in the program and coordinate with external stakeholders, such as the Department of the Treasury, as appropriate. (Recommendation 5) |
VA concurred with this recommendation. In a July 2025 update, VA stated that the Office of Integrated Veteran Care, in collaboration with the Office of Integrity and Compliance and financial stakeholders, is leveraging existing processes to regularly identify inherent fraud risks within the Foreign Medical Program. VA stated that the Foreign Medical Program regularly reports to a risk oversight committee and discusses risks, mitigation strategies, and monitoring activities. According to VA, committee members recommend and evaluate mitigation strategy effectiveness to reduce the likelihood of risk occurrence and review the effectiveness of ongoing monitoring activities to ensure current risk management protocols are functioning as intended. In an October 2025 update, VA provided a fraud risk assessment completed by its Internal Review and Oversight team. The assessment lacked evidence of coordination with stakeholders, a mitigation approach for the top risks, a comprehensive list of fraud risks, and description of the rationale supporting the decisions. VA also stated the agency coordinated with the Department of the Treasury, which confirmed the department does not have access to key documents to help assess fraud risks. Conducting regularly scheduled fraud risk assessments covering the five key elements of such assessments would help ensure that the Foreign Medical Program effectively prevents, detects, and responds to fraud.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, assess the likelihood and impact of inherent fraud risks in the program. (Recommendation 6) |
VA concurred with this recommendation. In a July 2025 update, VA stated that the Foreign Medical Program leadership team continues to monitor existing and potential risks and regularly assesses current and emerging risks. VA stated that the Foreign Medical Program is considering whether technological solutions exist to facilitate identification of the likelihood and impact of fraud risk in the program. In an October 2025 update, VA stated its Internal Review and Oversight team, Office of Integrated Veteran Care, and the Foreign Medical Program identified likelihood and impact scores of identified fraud risk as part of its fraud risk assessment. VA provided a copy of this fraud risk assessment, but it lacked evidence of coordination with stakeholders, a mitigation approach for the top risks, and description of the rationale supporting the decisions. Conducting regularly scheduled fraud risk assessments covering the five key elements of such assessments would help ensure that the Foreign Medical Program effectively prevents, detects, and responds to fraud.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, determine a fraud risk tolerance for the program. (Recommendation 7) |
VA concurred with this recommendation. In a July 2025 update, VA stated that the Office of Integrated Veteran Care is finalizing the identification of fraud risk tolerance for the Foreign Medical Program, and once identified, it will be reviewed with senior leadership. In an October 2025 update, VA provided a fraud risk tolerance statement that did not indicate an understanding of the concepts involved, instead suggesting that the Foreign Medical Program maintains a zero-tolerance approach to fraud. Programs should consider defining risk tolerances with an understanding of what is possible with the resources available, targeting for action those risks that are above a certain fraud risk threshold. Conducting regular fraud risk assessments covering the five key elements of such assessments would help ensure that the Foreign Medical Program effectively prevents, detects, and responds to fraud.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, examine the suitability of existing fraud controls and prioritize residual fraud risks in the program. (Recommendation 8) |
VA concurred with this recommendation. In a July 2025 update, VA stated that the Office of Integrated Veteran Care's Office of Internal Review and Oversight is assisting the Foreign Medical Program in conducting a business process inventory that will identify internal fraud controls, gaps, and any associated risks. VA expects testing of program fraud controls and the prioritization of any residual fraud risks to be completed by July 2026. In an October 2025 update, VA stated its Internal Review and Oversight team, Office of Integrated Veteran Care, and the Foreign Medical Program examined the suitability of existing fraud controls and prioritized residual fraud risks. VA provided documentation that identified control objectives for a variety of process areas, such as claims processing and auditing, but did not indicate how the controls will be operationalized nor the prioritization of residual fraud risks. Conducting regular fraud risk assessments covering the five key elements of such assessments would help ensure that the Foreign Medical Program effectively prevents, detects, and responds to fraud.
|
| Veterans Health Administration | The Under Secretary for Health should, in coordination with the Foreign Medical Program, document a fraud risk profile for the program. (Recommendation 9) |
VA concurred with this recommendation. As of January 2025, VA stated that the Office of Integrated Veteran Care, in collaboration with the Office of Integrity and Compliance and financial stakeholders, will continue advancing the development of a comprehensive internal control program and that this initiative will include a process to document a fraud risk profile. In a July 2025 update, VA stated that the Foreign Medical Program will review the results of a risk assessment survey once available. According to VA, coordination with stakeholders is ongoing to finalize and document a fraud risk profile for the Foreign Medical Program. In an October 2025 update, VA provided elements of a fraud risk profile developed by its Internal Review and Oversight team, Office of Integrated Veteran Care, and the Foreign Medical Program. VA stated the fraud risk profile includes evaluations of inherent and residual risk levels providing a clear picture of the raw exposure and impact of existing controls and mitigation measures. However, the fraud risk profile provided did not include all identified fraud risks nor assigned responsibilities and timing for risk mitigation strategies. Conducting regular fraud risk assessments covering the five key elements of such assessments would help ensure that the Foreign Medical Program effectively prevents, detects, and responds to fraud.
|
