Disease modeling: How Math Can Help In A Pandemic
The COVID-19 pandemic has brought new attention to models of infectious disease. These models are critical tools that scientists—including those from the Centers for Disease Control and Prevention (CDC)—use to anticipate health care needs and explore options for responding to an outbreak.
Today’s WatchBlog looks at the basics of infectious disease modeling, which we reviewed in a recent 2-page Spotlight. It also looks at our recent report on how federal agencies like the CDC use modeling, and how they might improve their use.
The many uses of models
Mathematical models are sets of equations that try to capture a complicated reality in a simplified form. No equation can encompass all of reality, so the idea is to capture enough of it to improve our ability to understand and predict.
In the case of COVID-19, sometimes that means using statistics about how the disease spreads in one place to predict what will happen in another. Such models, known as “statistical” models, have helped hospitals and governments prepare for things like surges in demand for intensive care unit beds and ventilators.
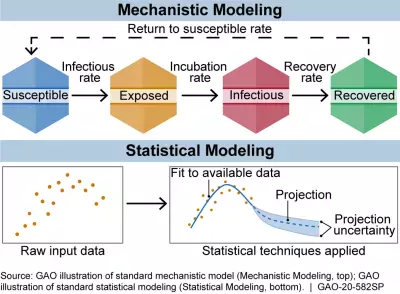
But prediction is not the only use for disease models. Some “mechanistic” models try to portray how diseases spread. One common version categorizes a hypothetical population by disease status—using terms like susceptible, exposed, infectious, or recovered—and then estimates how often people move from one category to another. These models can be particularly helpful in exploring what might happen under various policy scenarios.
For example, a COVID-19 model built by researchers at Imperial College London looked at a hypothetical scenario in which social distancing was not used. At one point, the model projected over 2 million U.S. deaths by October 2020. This estimate now seems inaccurate, but it was based on a scenario that, thankfully, did not come to pass.
This model proved valuable not by showing us what is going to happen, but what might have been. (For those who want more information about social distancing, we published a Spotlight on that, too.)
The figure below shows the 2 broad categories of infectious disease models: mechanistic models, which use scientific understanding of disease dynamics and human behavior, and statistical models, which rely only on patterns in the data.
The state of federal disease modeling
We also recently issued a report on federal modeling efforts for past outbreaks of three infectious diseases: Ebola, Zika, and pandemic influenza.
In this report, one of our key findings was that the CDC modelers did not always provide the details needed to reproduce their results. We recommended that they do so, because reproducibility provides a key check on scientific accuracy.
However, we also found that modelers at the CDC and elsewhere in the federal government largely followed GAO-identified commonly recognized modeling practices, despite often facing urgent outbreaks and shortages of the data they need. The evidence we found for the soundness of their work may be a reason for optimism amid the current pandemic.
Want to know more? Check out our Science & Tech Spotlight on infectious disease modeling, and our report on modeling at federal agencies, released in June 2020.
Comments on GAO’s WatchBlog? Contact blog@gao.gov.