Medicaid Program Integrity: Action Needed to Ensure CMS Completes Financial Management Reviews in a Timely Manner
Fast Facts
The Centers for Medicare & Medicaid Services (CMS) conducts financial management reviews to verify states' appropriate spending of federal Medicaid funds.
Since FY2016, CMS started 49 financial management reviews, usually focused on one state. As of June 2020, most reviews were still ongoing. Some states won't address the problems identified until the reviews are done, leaving federal and state dollars at risk for misspending.
What takes so long? CMS officials cite competing priorities, less staff, and the multi-step review process as contributing to the delay. We recommended setting time frames to ensure timely financial management reviews.
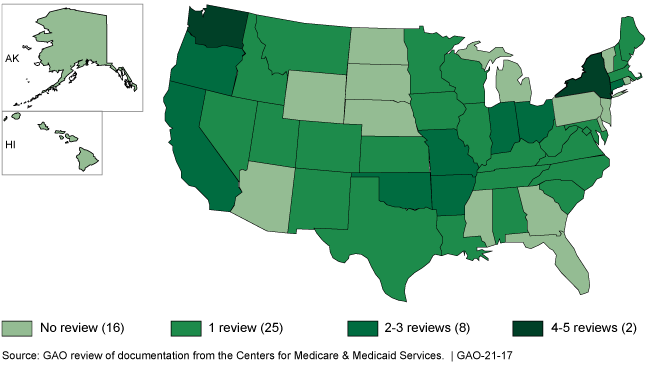
Number of Medicaid Financial Management Reviews by State, FYs 2016-2020
Highlights
What GAO Found
Since fiscal year 2016, the Centers for Medicare & Medicaid Services (CMS) has initiated 49 financial management reviews (FMR) to examine state Medicaid agencies' compliance with a variety of federal policies. These 49 FMRs frequently found one or more instances of states' non-compliance.
- CMS identified instances of non-compliance that had a financial impact totaling about $358 million.
- CMS identified internal control weaknesses and directed states to make changes to their Medicaid policies.
However, FMRs have not always examined topics or states that reflect the areas of highest expenditures. In 2018, GAO recommended that CMS improve its targeting of oversight resources. CMS agreed with this recommendation, but has not yet implemented it. In addition, CMS guidance generally expects draft FMR reports to be completed in the year they began. However, two-thirds of FMRs (26 of 39) initiated in fiscal years 2016 to 2019 were still under review in June 2020, which can delay state actions to address program vulnerabilities. CMS officials said that at least five states would not take actions—such as returning federal funds for unallowable expenditures—until they received a complete report.
Status of Financial Management Reviews (FMR) Initiated in Fiscal Years 2016 to 2019, as of June 2020

CMS officials cited competing priorities, decreased staff, and the agency's review process—which involves multiple steps and levels of review—as factors affecting their use of FMRs for oversight. CMS took steps during the course of GAO's review to complete FMRs that had been under review for several years. The agency has not established time frames for the completion of individual review steps or for its overall review of FMR reports. Developing and implementing such time frames would provide a tool to help monitor CMS's progress in completing FMRs and ensure prompt action on FMR findings.
Why GAO Did This Study
Over the last two decades, Medicaid—a joint, federal-state health care financing program for low-income and medically needy individuals—more than tripled in expenditures and doubled in enrollment. CMS estimates the program will continue to grow, exceeding $1 trillion in expenditures and 81 million enrollees in 2028. The size and growth of Medicaid present oversight challenges. CMS is responsible for assuring that states' Medicaid expenditures comply with federal requirements, and FMRs are one of its financial oversight tools. CMS generally directs its regional offices to conduct one focused FMR each year on an area of high risk within their regions, typically within one state.
GAO was asked to examine CMS's use of FMRs. In this report, GAO examines the extent to which CMS has used FMRs to oversee state Medicaid programs. GAO reviewed CMS documentation on FMR findings and their status, and resources assigned to FMRs and other financial review functions. GAO also interviewed CMS officials from all 10 regional offices and the central office, and assessed CMS's FMR policies and procedures against federal internal control standards.
Recommendations
CMS should develop and implement time frames to ensure the timely completion of FMRs. The Department of Health and Human Services concurred with our recommendation.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Centers for Medicare & Medicaid Services | The Administrator of CMS should develop and implement time frames to ensure that the agency completes FMRs in a timely manner. (Recommendation 1) |
The Department of Health and Human Services (HHS) concurred with this October 2020 recommendation (GAO-21-17). In December 2025, HHS stated that the implementation status for this recommendation is in progress and still open. In February 2025, HHS reported that the Centers for Medicare & Medicaid Services (CMS) was continuing to pursue strategies to ensure the timeliness of financial management reviews (FMR) including developing and implementing time frames for their completion. For example, in May 2021, HHS told us that CMS was establishing FMR field work start and end dates, deadlines for states to provide CMS with data and supporting documentation, and time frames for producing draft and final FMR reports.
|
