Department of Defense: Eating Disorders in the Military
Fast Facts
We looked at how the Department of Defense screens and provides treatment for eating disorders. These disorders have severe health effects and can significantly raise the risk of death. Many people with eating disorders may also have other mental health conditions such as anxiety.
While DOD screens new recruits for eating disorders, medical personnel may also detect these conditions during a servicemember's annual health screening. With DOD's health coverage, servicemembers and their dependents can get specialized care for eating disorders through civilian providers working in 166 eating disorder facilities across 32 states.
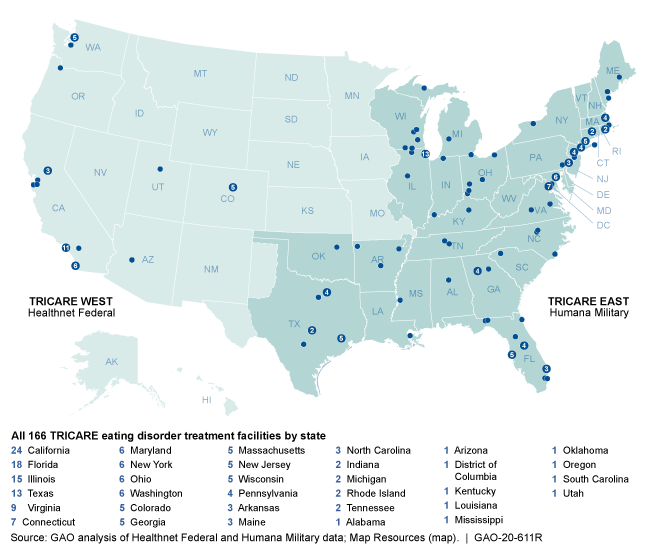
Facilities Where Eating Disorder Treatment Is Covered under the Department of Defense Health System, TRICARE, Spring 2020
Highlights
What GAO Found
The Department of Defense (DOD) screens for eating disorders for all applicants entering into the military but does not specifically screen servicemembers for eating disorders after entrance. However, after joining the military, servicemembers receive annual health screenings, and medical personnel may be able to diagnose eating disorders during in-person physical exams. Service branch behavioral health specialists told GAO that DOD medical personnel are trained to notice signs of eating disorders, such as changes in vital signs and emaciated appearance. DOD is examining ways to improve its screening of eating disorders in the military and recently expanded the available research funding for eating disorders in its Peer-Reviewed Medical Research Program (PRMRP).
DOD provides health care services to approximately 9.5 million eligible beneficiaries, including services to treat those diagnosed with eating disorders, through TRICARE, DOD’s regionally structured health care system. Servicemembers can obtain these services at military treatment facilities—referred to as direct care—or receive care purchased from civilian providers—referred to as purchased care. DOD officials told us that the specialized level of care necessary to treat eating disorders is available to TRICARE beneficiaries through purchased care, rather than direct care. The Defense Health Agency (DHA), which oversees the TRICARE program, uses two contractors to develop regional provider networks.
According to the two TRICARE contractors’ data for purchased care, as of spring 2020, there were 166 eating disorder facilities located in 32 states throughout the country and the District of Columbia. The facilities vary by geographic location, population served, and level of treatment provided:
- Geography: About half of the 166 facilities (79) are located in the following five states: California (24), Florida (18), Illinois (15), Texas (13), and Virginia (nine).
- Population: Of the 166 eating disorder facilities, over three-quarters provide treatment to both adult (132 facilities) and child and adolescent (132 facilities) populations.
- Level of Treatment: Most facilities provide inpatient hospitalization programs, which are for serious cases requiring medical stabilization (81 facilities); partial hospitalization, which are day programs providing treatment 5 to 7 days a week (133 facilities); or intensive outpatient programs, which are treatment programs providing therapy 2 to 6 days a week (107 facilities). About one-fifth of the facilities (35) provide residential treatment services, which are living accommodations providing intensive therapy and 24-hour supervision.
TRICARE contractors have met with some challenges entering into contracts with eating disorder treatment facilities in certain areas of the country, according to DHA officials and both contractors. However, both contractors told GAO they consider it their responsibility to ensure beneficiaries receive the care they need regardless of the location of the facility. No access-to-care complaints related to eating disorder treatment were reported by TRICARE beneficiaries, according to the most recent DHA data for years 2018 through 2019.
Why GAO Did This Study
Eating disorders are complex conditions affecting millions of Americans and involve dangerous eating behaviors, such as the restriction of food intake. They can have a severe impact on heart, stomach, and brain functionality, and they significantly raise the risk of mortality. Many with eating disorders also experience co-occurring conditions such as depression. Research has yielded a range of estimates of the number of servicemembers with an eating disorder, due to differences in research methods. For example, a 2018 DOD study concluded that servicemembers likely experienced eating disorders at rates that are comparable to rates in the general population, while other survey-based research suggested the number of servicemembers with eating disorders may be higher than those with a medical diagnoses of such disorders. The potential effects that eating disorders can have on the health and combat readiness of servicemembers and their dependents underscores the importance of screening and treating this population.
GAO was asked to provide information on eating disorders among servicemembers and their dependents. To describe how DOD screens for eating disorders among servicemembers, GAO reviewed DOD policies related to health screening and interviewed behavioral health specialists from the military branches. To understand approaches and challenges with implementing screening in a military environment, any planned or ongoing DOD-sponsored research related to this topic, and available eating disorder treatment, GAO interviewed representatives from the Eating Disorder Coalition, Uniformed Services University of Health Sciences, and the University of Kansas. To describe how DOD provides eating disorder treatment to servicemembers and their dependents, GAO interviewed DHA officials and TRICARE contractors and reviewed the TRICARE policy manual to identify the types of eating disorder diagnoses and treatments that are covered through direct and purchased care. GAO received data from the two TRICARE contractors related to the availability of eating disorder treatment services as of spring 2020.
For more information, contact Sharon Silas at (202) 512-7114 or Silass@gao.gov.
