Medicare Plan Finder: Usability Problems and Incomplete Information Create Challenges for Beneficiaries Comparing Coverage Options
Fast Facts
Medicare beneficiaries have many decisions to make when selecting their health and prescription drug coverage. Their choices affect their out-of-pocket costs and which providers they can see. The Medicare Plan Finder website is a primary source for comparing options.
Many officials who assist beneficiaries in selecting coverage—about three-quarters of those we surveyed—told us beneficiaries struggle with the website. They and others said it is difficult to navigate, contains complex terms, and lacks information needed to compare coverage options.
Medicare’s administrator plans to launch a redesigned website in August.
Screenshot of Medicare.gov's Medicare Plan Finder
Highlights
What GAO Found
The Medicare Plan Finder (MPF) website—a primary resource for comparing Medicare coverage options—is difficult for beneficiaries to use and provides incomplete information, according to stakeholders and research studies. These sources and directors of State Health Insurance Assistance Programs (SHIP) GAO surveyed—who assist beneficiaries with their Medicare coverage choices—reported that beneficiaries struggle with using MPF because it can be difficult to find information on the website and the information can be hard to understand. For example, MPF
requires navigation through multiple pages before displaying plan details,
lacks prominent instructions to help beneficiaries find information, and
contains complex terms that make it difficult for beneficiaries to understand information.
In response to GAO's survey, 73 percent of SHIP directors reported that beneficiaries experience difficulty finding information in MPF, while 18 percent reported that SHIP counselors experience difficulty.
User Difficulty Finding Information in Medicare Plan Finder, Reported by SHIP Directors, 2018
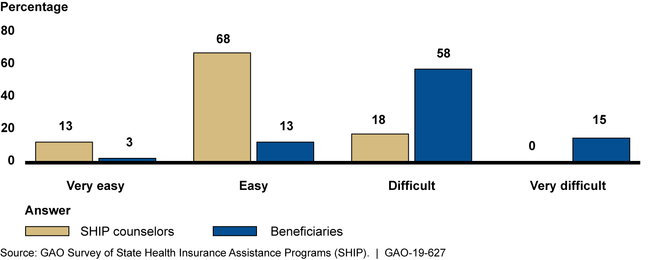
Note: Percentages do not round to 100 as some SHIP directors said they had no basis to respond.
Stakeholders and SHIP directors reported that MPF provides incomplete estimates of costs under original Medicare, making it difficult to compare original Medicare and Medicare Advantage (MA), the program's private heath plan alternative. Specifically, MPF's plan results pages do not integrate information on Medigap plans. (These plans help cover some of beneficiaries' out-of-pocket costs.) Seventy-five percent of the SHIP directors surveyed reported that the lack of Medigap information in MPF limits the ability of beneficiaries to compare original Medicare to MA.
The Centers for Medicare & Medicaid Services (CMS)—the agency that administers MPF—is aware of the difficulities beneficiaries face using MPF and is planning to launch a redesigned website in August 2019. According to CMS, redesigning MPF involves multiple iterations of changes and ongoing user testing, and CMS will know more about how well the redesigned MPF addresses user needs after it is used by beneficiaries.
Why GAO Did This Study
Medicare beneficiaries—more than 60 million as of 2019—have a series of decisions to make when selecting their Medicare health and prescription drug coverage. Beneficiaries must first choose between two main options for their Medicare coverage: either original fee-for-service Medicare or MA. Within these two options, beneficiaries have many additional choices, and they are permitted to change their coverage at least annually. These selections can be difficult due to the Medicare program's complexity and can have important implications for beneficiaries' out-of-pocket costs and access to providers.
According to CMS, the MPF website is intended to help beneficiaries make informed decisions regarding their health care and prescription drug coverage. However, some stakeholders have raised concerns that beneficiaries experience challenges using MPF to compare their Medicare coverage options.
GAO was asked to review MPF. This report examines what is known about the usability of MPF and the completeness of its information. GAO reviewed research and CMS documentation on MPF, and surveyed 51 directors of SHIP offices that have counselors who assist beneficiaries with Medicare decisions. Forty SHIP directors completed the survey, resulting in a 78 percent response rate. GAO also interviewed CMS officials and officials with 13 stakeholder groups, including seven beneficiary advocacy groups.
GAO provided a draft of this report to the Department of Health and Human Services. The department provided technical comments, which GAO incorporated as appropriate.
For more information, contact James Cosgrove at (202) 512-7114 or cosgrovej@gao.gov.
