Indian Health Service: Agency Faces Ongoing Challenges Filling Provider Vacancies
Fast Facts
Indian Health Service clinics don’t have enough doctors or nurses to provide quality and timely health care to American Indian and Alaska Native people. IHS data show an average vacancy rate for physicians, nurses, and other care providers of 25%.
IHS uses multiple strategies to recruit and retain providers, including offering financial incentives and housing. However, IHS has trouble matching local market salaries and does not have enough housing to meet the demand. One way the agency tries to fill vacancies is by hiring temporary providers, although officials said this is more costly and may result in less continuity of care.

Photo of the sign in front of an Indian Health Service building
Highlights
What GAO Found
Indian Health Service (IHS) data show sizeable vacancy rates for clinical care providers in the eight IHS geographic areas where the agency provides substantial direct care to American Indian/Alaska Native (AI/AN) people. The overall vacancy rate for providers—physicians, nurses, nurse practitioners, certified registered nurse anesthetists, certified nurse midwives, physician assistants, dentists, and pharmacists—was 25 percent, ranging from 13 to 31 percent across the areas.
Number of Provider Positions and Vacancy Rates by IHS Area, November 2017
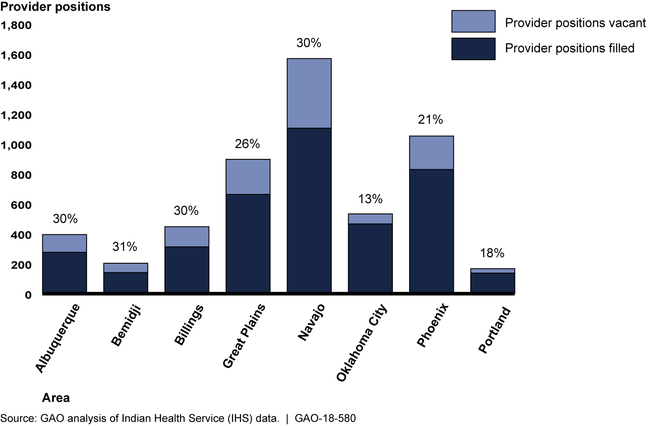
IHS officials told GAO that challenges to filling these vacancies include the rural location of many IHS facilities and insufficient housing for providers. Officials said long-standing vacancies have a negative effect on patient access, quality of care, and employee morale.
IHS uses multiple strategies to recruit and retain providers, including offering increased salaries for certain positions, but it still faces challenges matching local market salaries. IHS also offers other financial incentives, and has made some housing available when possible. In addition, IHS uses strategies, such as contracting with temporary providers, to maintain patient access to services and reduce provider burnout. Officials said these temporary providers are more costly than salaried employees and can interrupt patients' continuity of care. However, IHS lacks agency-wide information on the costs and number of temporary providers used at its facilities, which impedes IHS officials' ability to target its resources to address gaps in provider staffing and ensure access to health services across IHS facilities.
Why GAO Did This Study
IHS is charged with providing health care to AI/AN people who are members or descendants of 573 tribes. According to IHS, AI/AN people born today have a life expectancy that is 5.5 years less than all races in the United States, and they die at higher rates than other Americans from preventable causes. The ability to recruit and retain a stable clinical workforce capable of providing quality and timely care is critical for IHS. GAO was asked to review provider vacancies at IHS.
This report examines (1) IHS provider vacancies and challenges filling them; (2) strategies IHS has used to recruit and retain providers; and (3) strategies IHS has used to mitigate the negative effects of provider vacancies. GAO reviewed IHS human resources data for the provider positions that the agency tracks. GAO also reviewed policies, federal internal control standards, and legal authorities related to providers in federally operated IHS facilities. GAO interviewed IHS officials at the headquarters and area level and at selected facilities. GAO selected facilities based on variation in their number of direct care outpatient visits and inpatient hospital beds in 2014.
Recommendations
GAO recommends that IHS obtain, on an agency-wide basis, information on temporary provider contractors, including their associated cost and number of full-time equivalents, and use this information to inform decisions about resource allocation and provider staffing.
IHS concurred with GAO's recommendation.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Indian Health Service | The Director of IHS should obtain, on an agency-wide basis, information on temporary provider contractors, including their associated cost and number of full-time equivalents, and use this information to inform decisions about resource allocation and provider staffing. (Recommendation 1) |
In May 2021, IHS officials reported that they developed a contract provider cost tracking system and pilot tested it in February 2020. Since then, on a monthly basis, IHS area officials and facility employees upload contract provider costs into the tracking system. Officials at the Headquarters, area, and facility levels have used the data collected by the tracking system to inform decisions related to staffing and budget. This will allow IHS to target its resources to address gaps in provider staffing and ensure access to health services across IHS facilities.
|
