Medicaid: Demographics and Service Usage of Certain High-Expenditure Beneficiaries
Highlights
What GAO Found
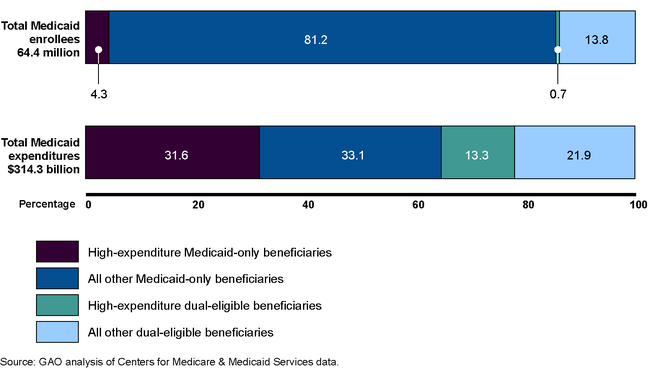
In fiscal year 2009, states spent nearly a third (31.6 percent) of all Medicaid expenditures on the most expensive Medicaid-only beneficiaries, who were 4.3 percent of total Medicaid beneficiaries. States spent another third (33.1 percent) on all other Medicaid-only beneficiaries, who represented 81.2 percent of total Medicaid beneficiaries. Among dual eligible beneficiaries, a similar pattern existed, with a small proportion of the population accounting for a disproportionate share of expenditures.
Percent of Total Medicaid Expenditures on Beneficiary Spending Groups, Fiscal Year 2009
Certain characteristics significantly increased the probability of being a high-expenditure Medicaid-only beneficiary. Specifically, the results of GAO's analyses indicate that the probability of being a high-expenditure Medicaid-only beneficiary was:
- 24.4 percent for those residing in a long-term care facility,
- 20.8 percent for those with human immunodeficiency virus/acquired immunodeficiency syndrome,
- 18.3 percent for those with disabilities, and
- 13.3 percent for new mothers or infants.
Overall, hospital services and long-term services and supports in non-institutional and institutional settings comprised nearly 65 percent of the total expenditures for high-expenditure Medicaid-only beneficiaries, with smaller proportions for drugs, payments to managed care organizations and premium assistance, and non-hospital acute care. In contrast to high-expenditure beneficiaries, payments to managed care organizations and premium assistance comprised 57.2 percent of total expenditures for all other Medicaid-only beneficiaries.
HHS provided technical comments on a draft of this report, which were incorporated as appropriate.
Why GAO Did This Study
Medicaid is an important source of health coverage for millions of low-income individuals. Research on Medicaid has demonstrated that a small percentage of beneficiaries account for a disproportionately large share of Medicaid expenditures. Understanding states' expenditures for high-expenditure populations—both those dually eligible for Medicare and Medicaid, and those who are Medicaid-only—could enhance efforts to manage Medicaid expenditures.
GAO was asked to examine the demographics and service usage of Medicaid beneficiaries, particularly those who are not eligible for Medicare. This report examines high-expenditure Medicaid-only beneficiaries, considering (1) states' spending on them compared with all other Medicaid beneficiaries; (2) their key characteristics; and (3) their service usage compared with all other Medicaid-only beneficiaries.
GAO analyzed beneficiary and expenditure data from the Medicaid Statistical Information System Annual Person Summary File for 2009, the most recent year available at the time GAO conducted its work. GAO defined high-expenditure beneficiaries as those with total expenditures in the top 5 percent of expenditures within each state. GAO combined these data at a national level, and analyzed the characteristics associated with being a high-expenditure beneficiary, the probability of being a high-expenditure Medicaid beneficiary, and what services contributed to high expenditures.
For more information, contact Carolyn L. Yocom at (202) 512-7114 or YocomC@gao.gov.
