Pediatric Trauma Centers: Availability, Outcomes, and Federal Support Related to Pediatric Trauma Care
Fast Facts
More children die of injury each year than from all other causes combined. When children are severely injured in an event such as a car crash, where do they go to get care?
Although most traumatic injuries are treated in hospital emergency departments, hospitals may not have the resources needed to treat injured children. For example, they may lack specially sized medical equipment. Pediatric trauma centers, however, have these resources.
We found that 57 percent of the nation's 74 million children lived within 30 miles of a pediatric trauma center that can treat pediatric injuries, regardless of severity.
Estimated Percentage of Children Who Lived within 30 Miles of a Pediatric Trauma Center That Can Treat All Injuries, by State, 2011-2015
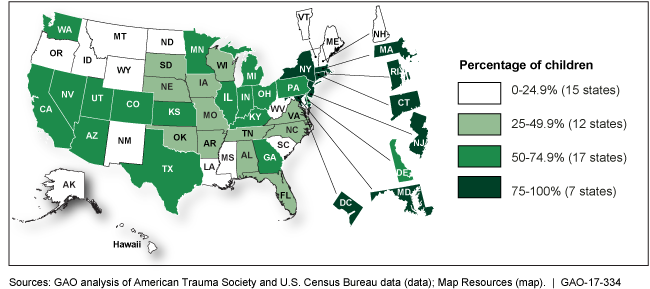
Map of the percentage of children within 30 miles of pediatric trauma center that can treat all injuries
Highlights
What GAO Found
GAO estimates that 57 percent of the 73.7 million children in the United States during the period 2011-2015 lived within 30 miles of a pediatric trauma center that can treat all injuries regardless of severity. Among states, the proportion of children who lived within 30 miles of these pediatric trauma centers varied widely. In areas without pediatric trauma centers, injured children may have to rely on adult trauma centers or less specialized hospital emergency departments for initial trauma care. Some studies GAO reviewed, including nationwide studies, found that children treated at pediatric trauma centers have a lower mortality risk compared to children treated at adult trauma centers and other facilities, while other state-level studies GAO reviewed found no difference in mortality. Further, some studies GAO reviewed and stakeholders GAO interviewed suggest that more information is needed on outcomes other than mortality for children treated at pediatric trauma centers because mortality can be a limited outcome measure, as overall mortality is low among severely injured children.
Estimated Percentage of Children Who Lived within 30 Miles of a High-Level Pediatric Trauma Center, by State, 2011-2015
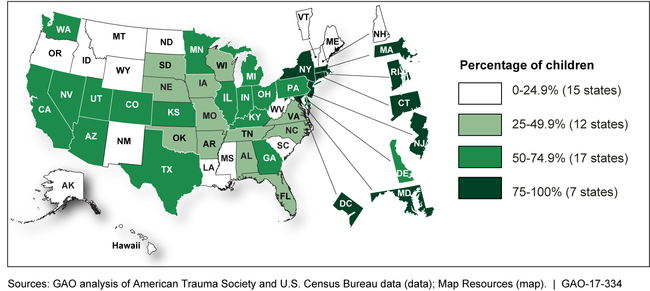
Note: High-level pediatric trauma centers have the resources to treat all injured children, regardless of injury severity.
Two agencies within the Department of Health and Human Services (HHS)—the Health Resources and Services Administration (HRSA) and the National Institutes of Health (NIH)—have grant programs and other activities that support hospital-based pediatric trauma care. For example, HRSA's Emergency Medical Services for Children Program provides grants to integrate pediatric emergency care—which encompasses care for both traumatic injury and illness—into states' larger emergency medical services systems. GAO also found that federal activities related to hospital-based pediatric trauma care and other emergency care are coordinated through an interagency group and arrangements among agencies. For example, HRSA and NIH staff participate in the Council on Emergency Medical Care, an interagency group established to coordinate emergency care activities across the federal government by promoting information sharing and policy development.
Why GAO Did This Study
Pediatric trauma—a severe and potentially disabling or life threatening injury to a child resulting from an event such as a motor vehicle crash or a fall—is the leading cause of disability for children in the United States. More children die of injury each year than from all other causes combined. GAO was asked to examine issues related to pediatric trauma care.
This report examines (1) what is known about the availability of trauma centers for children and the outcomes for children treated at different types of facilities, and (2) how, if at all, federal agencies are involved in supporting pediatric trauma care and how these activities are coordinated. GAO analyzed data on the number of pediatric and adult trauma centers in the United States relative to the pediatric population under 18 years of age. GAO used 2015 data on trauma centers from the American Trauma Society's Trauma Information Exchange Program and 5-year population estimates for 2011-2015 from the U.S. Census Bureau's American Community Survey, which were the latest available data at the time of GAO's analysis. GAO also reviewed the existing peer-reviewed, academic literature on outcomes for pediatric trauma patients, interviewed stakeholder group representatives and federal agency officials involved in activities related to hospital-based pediatric trauma care, and reviewed available agency documentation.
HHS provided technical comments on a draft of this report, which GAO incorporated as appropriate.
For more information, contact Marcia Crosse at (202) 512-7114 or crossem@gao.gov.
