The Role and Risk of Herd Immunity When It Comes to COVID-19
As the COVID-19 pandemic continues, the concept of herd immunity is coming into sharper focus. But with limited information available on critical aspects of COVID-19, the concept remains a murky one.
Today’s WatchBlog looks at our recent Spotlight on the complexities of herd immunity.
What is herd immunity?
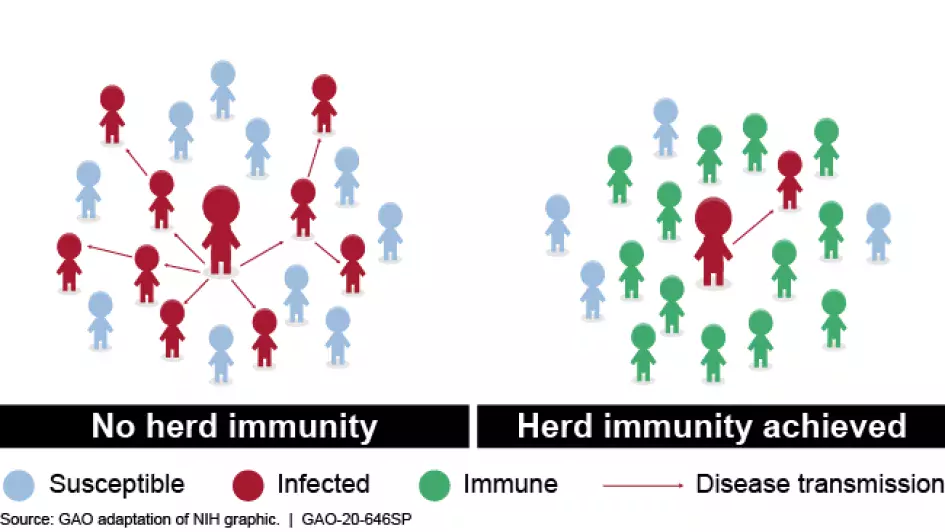
When a large enough portion of a population—say 70-90%—develops an immunity to a disease, that population is said to have achieved herd immunity. Establishing herd immunity reduces the likelihood that a non-immune person will be infected by the disease because they are less likely to come into contact with an infected person.
Once achieved, herd immunity could potentially slow down or stop the spread of COVID-19, support economic recovery, and restore medical capacity. However, achieving herd immunity in the absence of vaccines or treatments could also mean more deaths.
Why is it challenging to understand?
While data on previous disease outbreaks is available, we don’t yet have crucial data on COVID-19’s spread or severity. Consequently, researchers cannot say for certain when herd immunity is reached or, critically, how many lives might be lost when it is.
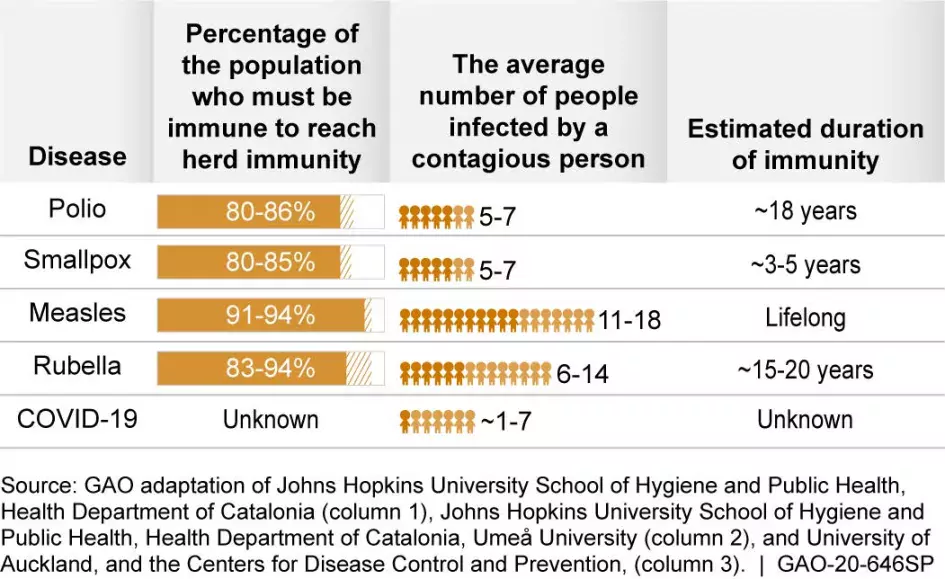
For instance, in order to determine when herd immunity will be reached, we need to know how contagious the disease is—which is affected by factors like how many susceptible people an infected person can infect. While researchers have developed estimates for how contagious COVID-19 is, uncertainties about case reporting and the accuracy of testing make this calculation difficult.
Other challenges include determining how long immunity to the disease might last. While analyses of related coronaviruses have shown that infection can provide some level of immunity, such immunity did not appear to last longer than a year.
What are the risks?
Immunity generally develops either through infection (natural immunity) or vaccination (resulting in vaccine-induced immunity), both of which carry high costs.
Achieving natural immunity, an unfavorable outcome by any measure, would mean exposing susceptible groups to a debilitating and potentially fatal disease—meaning more people could die in the process of achieving herd immunity.
Worse still, outbreaks may still occur when herd immunity is achieved because immunity may not be uniform across the general population. For example, contact among non-immune people may enable the disease to spread.
In the end, vaccine-induced herd immunity remains the more desirable goal, but, with challenges persisting in slowing the spread of COVID-19, natural disease progression may continue and with it, more deaths.
To learn more about herd immunity, check out our Science & Tech Spotlight on the topic.
-
Comments on GAO’s WatchBlog? Contact blog@gao.gov.
GAO Contacts
Related Products

GAO's mission is to provide Congress with fact-based, nonpartisan information that can help improve federal government performance and ensure accountability for the benefit of the American people. GAO launched its WatchBlog in January, 2014, as part of its continuing effort to reach its audiences—Congress and the American people—where they are currently looking for information.
The blog format allows GAO to provide a little more context about its work than it can offer on its other social media platforms. Posts will tie GAO work to current events and the news; show how GAO’s work is affecting agencies or legislation; highlight reports, testimonies, and issue areas where GAO does work; and provide information about GAO itself, among other things.
Please send any feedback on GAO's WatchBlog to blog@gao.gov.