Protecting Nursing Home Residents from Infections like COVID-19
Recent COVID-19 related deaths at nursing homes have raised concerns about the health and safety of the nation’s 1.4 million residents living in these facilities.
In today’s WatchBlog, we look at the federal role in protecting nursing home residents and our recent report that identified ongoing gaps in this effort that pre-date the coronavirus pandemic.
Nursing home infection control
There are about 15,500 nursing homes in the United States. Federal standards require that these facilities establish and maintain infection prevention and control programs.
While the Centers for Medicare & Medicaid Services is responsible for ensuring that these facilities have programs and safety measures in place, it relies on state agencies to conduct surveys and investigations of facilities to ensure nursing homes comply with federal standards.
Deficiencies in meeting these standards can include situations where, for example, nursing home staff did not regularly use proper hand hygiene or failed to implement preventive measures during an infectious disease outbreak like isolating sick residents. Many of these practices can be critical to preventing the spread of infectious disease, including COVID-19.
What we found
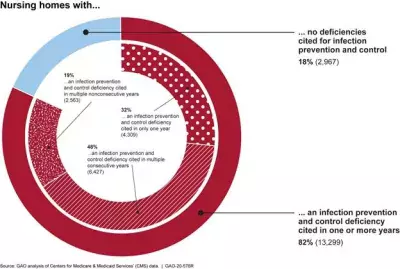
Our review of nursing homes, which pre-dated the COVID-19 pandemic, looked at data from Medicare & Medicaid and showed that infection prevention and control deficiencies were widespread among most nursing homes and often persistently found over multiple years. Infection prevention and control were the most commonly cited deficiencies in surveyed nursing homes. Between 2013 and 2017, 82% (13,299) of nursing homes were cited with an infection prevention control deficiency in one or more years. About 48% (6,327) of those nursing homes had multiple consecutive years of citations for deficiencies.
In each individual year from 2013 through 2017, the percent of surveyed nursing homes with an infection prevention and control deficiency ranged from 39 percent to 41 percent. In 2018 and 2019, we found that this continued with about 40 percent of surveyed nursing homes having an infection prevention and control deficiency cited each year.
We also found that in each year from 2013 through 2017, 99% of the infection prevention and control deficiencies were classified by state surveyors as “not severe.” As a result Medicare & Medicaid enforcement actions against nursing homes were only taken for 1% of these deficiencies. Furthermore, 67 percent of these infection prevention and control deficiencies classified as “not severe” did not have any enforcement actions imposed or implemented, and 31 percent had enforcement actions imposed but not implemented—meaning the nursing home likely had an opportunity to correct the deficiency before an enforcement action was imposed.
To learn more about our findings, tune in to our podcast with John Dicken, a director in our Health Care team.
The figure below shows the number of nursing homes with cited deficiencies in multiple years, between 2013 and 2017.
Note: CMS restructured its deficiency code system beginning on November 28, 2017, and, due to these coding changes, we did not analyze CMS data cited by surveyors from November 28, 2017, through December 31, 2017. Percentages may not add to 100 due to rounding.
Help from the Cares Act
The Coronavirus Aid, Relief, and Economic Security (CARES) Act has provided $200 million to CMS to prevent, prepare for, and respond to the coronavirus. Of that money, Congress has directed CMS to use at least $100 million on nursing home facilities in localities where the coronavirus has spread. Further, since the COVID-19 pandemic, HHS has taken a number of actions, including targeting nursing home inspections on infection prevention and control, providing new guidance for nursing homes, and enhancing reporting of nursing home infections.
To learn more about these issues, as well as how the federal government is responding to COVID-19, check out our website.
- Comments on GAO’s WatchBlog? Contact blog@gao.gov
GAO Contacts
Related Products

GAO's mission is to provide Congress with fact-based, nonpartisan information that can help improve federal government performance and ensure accountability for the benefit of the American people. GAO launched its WatchBlog in January, 2014, as part of its continuing effort to reach its audiences—Congress and the American people—where they are currently looking for information.
The blog format allows GAO to provide a little more context about its work than it can offer on its other social media platforms. Posts will tie GAO work to current events and the news; show how GAO’s work is affecting agencies or legislation; highlight reports, testimonies, and issue areas where GAO does work; and provide information about GAO itself, among other things.
Please send any feedback on GAO's WatchBlog to blog@gao.gov.