Stopping Antibiotic Resistance Before It Gets to Our Plates
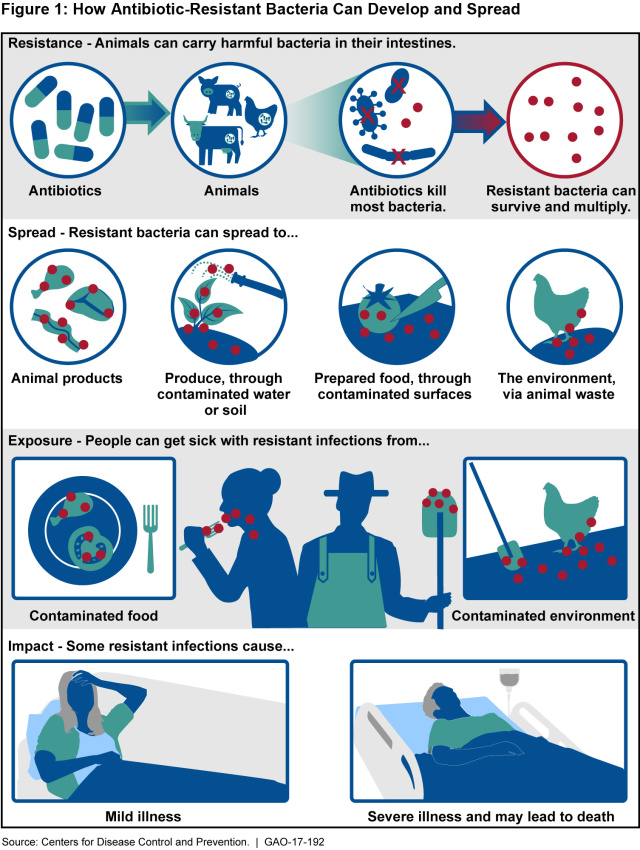
(Excerpted from GAO-17-192)
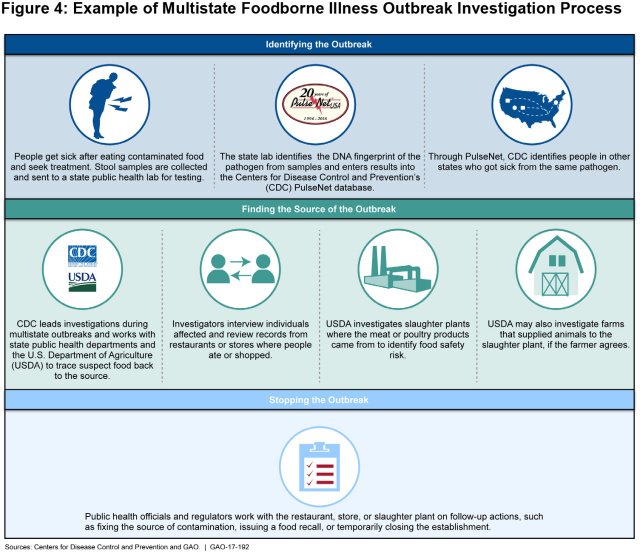
Looking for the Source of the Problem The Department of Health and Human Services and the U.S. Department of Agriculture are primarily responsible for ensuring the safety of the food supply, including the safe use of antibiotics in food animals. If a multistate foodborne illness outbreak does occur, HHS’s Centers for Disease Control and Prevention leads an investigation—in collaboration with USDA and state agencies—to trace the outbreak back to its source. These investigations may involve looking into farms, slaughter processing plants, or other points where bacteria from food animals can be transferred to the human population.(Excerpted from GAO-17-192)
In 2014, USDA established procedures to assess the root cause of foodborne illness outbreaks—potentially involving on-farm investigations to identify factors that may lead to antibiotic resistance. However, following a 2015 outbreak of antibiotic-resistant salmonella, no such on-farm investigation occurred because stakeholders could not agree on whether one was needed. We recommended that USDA, in coordination with the CDC and other stakeholders, develop a framework to help them decide when to conduct an on-farm investigation. To learn more—including how other countries manage the use of antibiotics in food animals—check out our full report.- Questions on the content of this post? Contact John Neumann at neumannj@gao.gov.
- Comments on GAO’s WatchBlog? Contact blog@gao.gov.

GAO's mission is to provide Congress with fact-based, nonpartisan information that can help improve federal government performance and ensure accountability for the benefit of the American people. GAO launched its WatchBlog in January, 2014, as part of its continuing effort to reach its audiences—Congress and the American people—where they are currently looking for information.
The blog format allows GAO to provide a little more context about its work than it can offer on its other social media platforms. Posts will tie GAO work to current events and the news; show how GAO’s work is affecting agencies or legislation; highlight reports, testimonies, and issue areas where GAO does work; and provide information about GAO itself, among other things.
Please send any feedback on GAO's WatchBlog to blog@gao.gov.