Electronic Health Information: HHS Needs to Improve Communications for Breach Reporting
Fast Facts
Health IT systems can enhance health care delivery and empower providers to make informed decisions about patient health. But these systems may be vulnerable to breaches.
The Department of Health and Human Services sets standards for protecting electronic health information and enforces compliance with them. Health care providers, health plans, their business associates, and other entities are required to report breaches to HHS.
The HHS Office of Civil Rights manages the breach reporting process, but it lacks a way for entities to provide feedback on it. This feedback could help improve the process.
Our recommendation addresses this issue.
Health Data Breaches Reported to HHS, 2015 to 2021
Highlights
What GAO Found
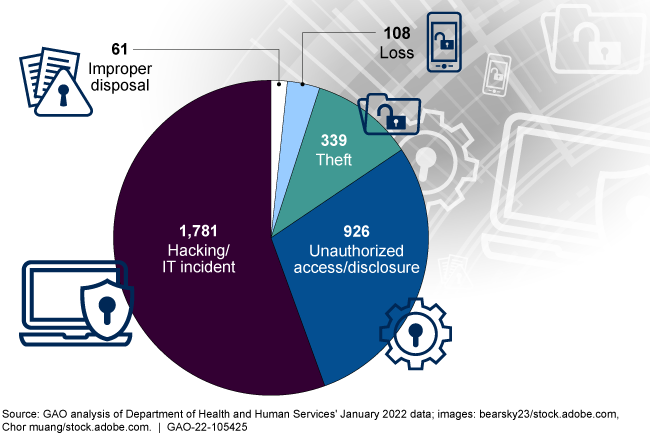
Since 2015, the Department of Health and Human Services (HHS) has seen an increase in reported breaches while the number of affected individuals has varied each year from approximately 5 to 113 million. Such breaches of health information involve the unauthorized (intentional or unintentional) exposure, disclosure, or loss of an individual's identifiable health information. The figure shows the number of breaches reported by various covered entities from 2015 through 2021.
Figure: The Number of Breaches Involving Unsecured Protected Health Information (PHI) from 2015 to 2021
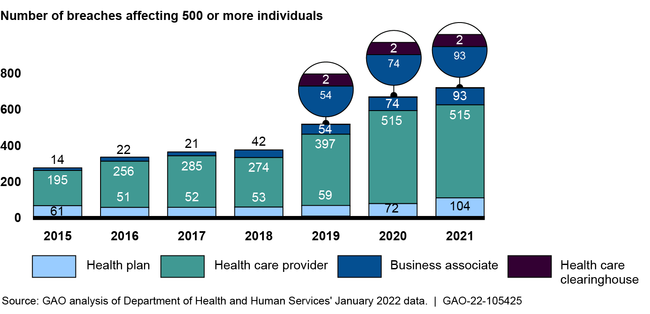
*Note: Business associates are entities that perform certain functions or activities that involve the use or disclosure of PHI on behalf of, or provides services to, a covered entity. Health care clearinghouses are entities that process nonstandard data elements of health information they receive from another entity into standard data elements or vice versa.
The HHS Office for Civil Rights (OCR), the unit responsible for enforcing the Health Insurance Portability and Accountability Act (HIPAA) standards, has taken steps to establish a process on whether entities implemented recognized security practices. A law enacted in January 2021 required HHS, as part of its enforcement activities, to consider whether covered entities had implemented such practices. In response, OCR established standard operating procedures for its investigators, published a request for information to seek public comments on implementation of security practices, and is conducting outreach to the health care sector. OCR expects to finalize the process no later than the summer of 2022.
OCR is charged with implementing and enforcing the HIPAA Privacy, Security and Breach Notification Rules, including the development and management of the breach reporting process. However, OCR does not have a method for covered entities to provide feedback on the breach reporting process, nor did the office indicate that it had plans to develop one. Without a clear mechanism to provide feedback to OCR, covered entities and business associates can face challenges during the breach reporting process. Further, soliciting feedback on the breach reporting process could help OCR improve aspects of the process.
Why GAO Did This Study
The use of IT allows health care providers and others to share health care information electronically, which enhances care delivery, public health and research; and empowers providers to make informed decisions regarding patient health.
HHS sets and enforces standards for protecting electronic health information. To implement the provisions of HIPAA, HHS issued regulations that govern PHI transmitted or maintained by covered entities, such as health plans and health care providers, and their business associates.
GAO was asked to review covered entities' required reporting to HHS on data breaches. This report examines (1) the number of breaches and affected individuals reported to HHS since 2015; (2) the extent to which HHS established a review process to assess whether covered entities had implemented recognized security practices; and (3) the extent to which improvements can be made related to HHS's breach reporting requirements.
To do so, GAO reviewed privacy and information security laws; analyzed HHS documentation, policies, and procedures; and interviewed cognizant OCR officials. GAO also surveyed HIPAA covered entities and business associates.
Recommendations
GAO is making one recommendation to HHS to establish a feedback mechanism to improve the effectiveness of its breach reporting process. HHS concurred with GAO's recommendation and described actions it would take to address it.
Recommendations for Executive Action
| Agency Affected | Recommendation | Status |
|---|---|---|
| Department of Health and Human Services | The Secretary of HHS should ensure that OCR establishes a mechanism for covered entities and business associates to provide feedback on OCR's breach reporting process. (Recommendation 1) |
Closed – Implemented
In February 2023, in response to our recommendation, we verified that HHS sends a reply email to every HIPAA breach report of unsecured protected health information. This email includes an email address, which is posted on OCR's website, that the reporting organizations can use to provide feedback about the HIPAA Breach Notification process. In addition, HHS has established a mailbox with a designated employee that is responsible for receiving covered entity and business associate feedback and questions regarding the breach reporting process. Accordingly, by creating these mechanisms to solicit feedback on the breach reporting process, HHS has an increased likelihood that it can improve or simplify aspects of the process and decrease long lapses of communication during ongoing breach reporting investigations.
|
