Rural Hospital Closures: Number and Characteristics of Affected Hospitals and Contributing Factors
Fast Facts
Has there been an increase in U.S. rural hospital closures?
Yes. From 2013 to 2017, 64 rural hospitals closed, more than twice as many as during the previous 5-year period.
What types of rural hospitals closed?
Rural hospital closures disproportionately occurred in the South, among for-profit hospitals, and among Medicare Dependent Hospitals—small rural hospitals with Medicare beneficiaries accounting for a certain percentage of their business.
Why have rural hospitals closed?
Financial distress. Multiple factors have exacerbated this, including a decrease in patients seeking inpatient care and across-the-board Medicare payment reductions.

Photo of a hospital sign directing people where to go for services.
Highlights
What GAO Found
The Department of Health and Human Services (HHS) administers multiple payment policies and programs that provide financial support for rural hospitals and funds research centers to monitor closures and study access. Among the payment policies administered by HHS are special payment designations for rural hospitals in which rural hospitals that meet certain criteria receive higher reimbursements for hospital services than they otherwise would receive under Medicare's standard payment methodology. HHS-funded research centers monitor rural hospitals' profitability and other financial indicators, and study access to facilities and specific services. HHS uses the results of monitoring activities to inform future areas of research and disseminate information.
GAO's analysis of data from HHS and an HHS-funded research center shows that 64 rural hospitals closed from 2013 through 2017. This represents approximately 3 percent of all the rural hospitals in 2013 and more than twice the number of closures of the prior 5-year period. GAO's analysis further shows that rural hospital closures disproportionately occurred in the South, among for-profit hospitals, and among hospitals that received the Medicare Dependent Hospital payment designation, one of the special Medicare payment designations for rural hospitals.
Percentage of Rural Hospitals in 2013 Relative to Percentage of Rural Hospital Closures from 2013 through 2017, by Selected Characteristics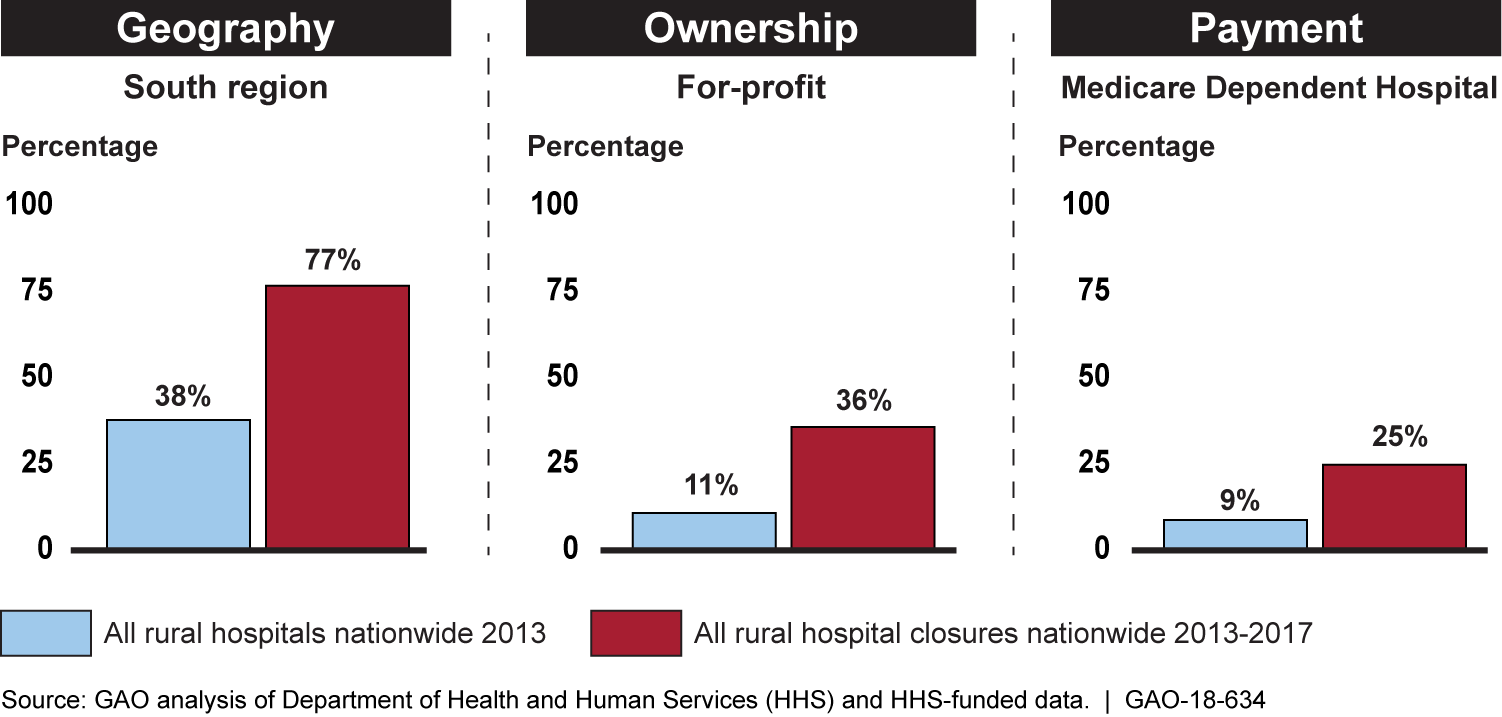
According to literature GAO reviewed and stakeholders GAO interviewed, rural hospital closures were generally preceded and caused by financial distress. In particular, rural hospitals that closed typically had negative margins that made it difficult to cover their fixed costs. According to these sources, financial distress has been exacerbated in recent years by multiple factors, including the decrease in patients seeking inpatient care and across-the-board Medicare payment reductions. In contrast, according to the literature GAO reviewed and stakeholders GAO interviewed, rural hospitals located in states that increased Medicaid eligibility and enrollment experienced fewer closures.
Why GAO Did This Study
Research has shown that hospital closures can affect rural residents' access to health care services and that certain rural residents—particularly those who are elderly and low income—may be especially affected by rural hospital closures.
This report describes (1) how HHS supports and monitors rural hospitals' financial viability and rural residents' access to hospital services and (2) the number and characteristics of rural hospitals that have closed in recent years and what is known about the factors that have contributed to those closures.
GAO reviewed documents and interviewed officials from HHS and HHS-funded research centers; analyzed data compiled by HHS and an HHS-funded research center, with a focus on 2013 through 2017—the most recent year with complete data; reviewed relevant literature; and interviewed experts and stakeholders. GAO identified hospitals as rural if they met the Federal Office of Rural Health Policy's definition of rural.
GAO provided a draft of this report to HHS for comment. The Department provided technical comments, which GAO incorporated as appropriate.
For more information, contact James Cosgrove at (202) 512-7114 or cosgrovej@gao.gov.
