Medicaid: Efforts to Exclude Nonemergency Transportation Not Widespread, but Raise Issues for Expanded Coverage
Highlights
What GAO Found
States' efforts to exclude nonemergency medical transportation (NEMT) benefits from enrollees who are newly eligible for Medicaid under the Patient Protection and Affordable Care Act (PPACA) are not widespread. Of the 30 states that expanded Medicaid as of September 30, 2015, 25 reported that they did not undertake efforts to exclude the NEMT benefit for newly eligible enrollees, 3 states reported pursuing such efforts, and 2 states—New Jersey and Ohio—did not respond to GAO's inquiry. However, the Centers for Medicare & Medicaid Services (CMS), within the Department of Health and Human Services (HHS), indicated that neither New Jersey nor Ohio undertook efforts to exclude the NEMT benefit.
State-Reported Actions to Exclude Medicaid's Nonemergency Medical Transportation (NEMT) Benefit for Newly Eligible Enrollees, September 2015
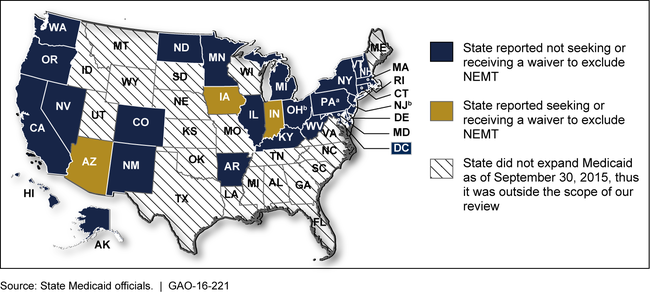
aAs part of Pennsylvania's efforts to expand Medicaid, the state received approval to exclude the NEMT benefit for its newly eligible enrollees; however, the state did not implement this exclusion.
bCMS provided information about New Jersey and Ohio's efforts related to the NEMT benefit.
Two of the three states pursuing efforts to exclude the NEMT benefit—Indiana and Iowa—have received waivers from CMS to exclude the benefit, and are in different stages of evaluating the effect these waivers have on enrollees' access to care.
Indiana's draft evaluation design describes plans to survey enrollee and provider experiences to assess any effect from excluding the NEMT benefit.
Iowa's evaluation largely found comparable access between enrollees with and without the NEMT benefit; however, it also found that newly eligible enrollees beneath the federal poverty level tended to need more transportation assistance or have more unmet needs than those with higher incomes.
Officials from the groups that GAO interviewed identified potential implications of excluding the NEMT benefit, such as a decrease in enrollee access to services and an increase in the costs of coverage. For example, nearly all of the groups indicated that excluding the NEMT benefit would impede access to services, particularly for those living in rural areas, as well as those with chronic health conditions.
Why GAO Did This Study
Medicaid, a federal-state health financing program for certain low-income individuals, offers NEMT benefits to individuals who are unable to provide their own transportation to medical appointments. This benefit can be an important safety net for program enrollees as research has identified the lack of transportation as affecting Medicaid enrollees' access to services. Under PPACA, states can opt to expand eligibility for Medicaid to certain adults. However, some states have excluded the NEMT benefit for these newly eligible enrollees by obtaining a waiver of the requirement under the authority of a Medicaid demonstration project.
GAO was asked to explore state efforts to exclude the NEMT benefit for newly eligible Medicaid enrollees, and the potential implications of such efforts. This report examines (1) the extent to which states have excluded this benefit for newly eligible enrollees, and (2) the potential implications of such efforts on enrollees' access to services.
GAO contacted the 30 states that expanded Medicaid under PPACA as of September 30, 2015; reviewed relevant documents and interviewed officials in the 3 states that have taken efforts to exclude the NEMT benefit; reviewed prior research on transportation for disadvantaged populations; and interviewed officials from CMS, the federal agency that oversees Medicaid, and 10 research and advocacy groups based on referrals from subject-matter experts and knowledge of the NEMT benefit.
HHS provided technical comments on a draft of this report, which GAO incorporated as appropriate.
For more information, contact Carolyn L. Yocom at (202) 512-7114 or yocomc@gao.gov or Mark L. Goldstein at (202) 512-2834 or goldsteinm@gao.gov.
