Medicaid: Service Utilization Patterns for Beneficiaries in Managed Care
Highlights
What GAO Found
Based on GAO's analysis of 2010 encounter data reported by 19 states, the number of professional services utilized by adult beneficiaries ranged from about 13 to 55. For children, the number of professional services utilized per beneficiary was lower, ranging from about 6 to 16 among the 19 states. Professional services included four categories of services: (1) evaluation and management (E/M) services, such as office visits and emergency room and critical care services; (2) procedural services, such as surgery and ophthalmology; (3) ancillary services, such as pathology and lab services; and (4) other professional services, such as oxygen therapy.
Adult and Child Professional Service Utilization in Selected States, 2010
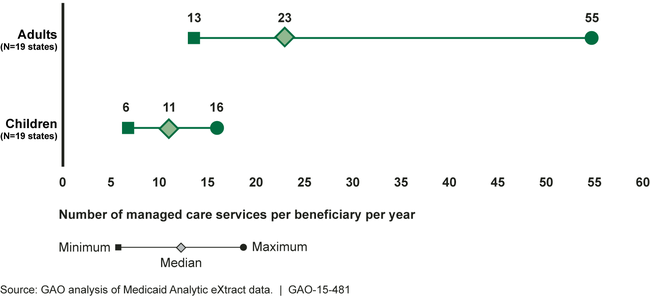
States varied considerably in how service utilization was distributed within service categories. For example, of total services,
adult per beneficiary utilization of ancillary services ranged from 37 percent in Rhode Island to 65 percent in Washington and Illinois; and
child per beneficiary utilization of E/M services ranged from 29 percent in Minnesota to 45 percent in Georgia and Rhode Island.
Service utilization for both adult and child beneficiaries also varied by the length of enrollment. When compared with beneficiaries enrolled for a full year, total service utilization for adults was 2 to 78 percent higher for partial-year beneficiaries—those enrolled in a comprehensive managed care plan for less than the full year—in slightly more than half of selected states. For children in all but one selected state, service utilization was 4 to 44 percent higher for partial-year beneficiaries compared with full-year beneficiaries.
Why GAO Did This Study
Medicaid, a federal-state health financing program for low-income and medically needy individuals, covered 65 million beneficiaries at an estimated cost of $508 billion in fiscal year 2014. More than half of Medicaid beneficiaries are enrolled in managed care plans, a health care delivery model where states contract with managed care organizations to provide covered services for a set cost. Historically, states have submitted relatively unreliable managed care service utilization data, also known as encounter data, to the Centers for Medicare & Medicaid Services, the federal agency that oversees Medicaid. However, recent evidence suggests that encounter data may be improving. Information on beneficiaries' service utilization could serve as a baseline for future analyses of utilization trends over time. GAO was asked to examine the level of services provided to these beneficiaries. In this report, GAO describes what encounter data indicate about the service utilization of Medicaid beneficiaries in managed care plans.
To do this work, GAO analyzed state-reported data included in CMS's 2010 Medicaid Analytic eXtract data and determined that 19 states had data that were reliable for its purposes, but excluded the remaining 31 states and the District of Columbia. For these 19 states, GAO calculated service utilization rates for adult and child beneficiaries enrolled in comprehensive managed care plans by state, service category, and length of enrollment. GAO received technical comments on a draft of this report from HHS and incorporated them as appropriate.
For more information, contact Carolyn Yocom at (202) 512-7114 or yocomc@gao.gov.
